Does Medicaid Cover ABA Therapy
Table of Contents
Understanding Medicaid Coverage for ABA Therapy
One of the most common questions we hear from families is, does medicaid cover aba therapy? At Heart Core ABA, we understand how crucial this is for accessing essential support for children with autism spectrum disorder. As a federal-state program, Medicaid provides health coverage to low-income families, making it a lifeline for many seeking affordable care. While federal guidelines under the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) services mandate coverage for medically necessary treatments like ABA in most cases, specifics for Medicaid ABA therapy coverage can vary by state.
Applied Behavior Analysis, or ABA therapy, is an evidence-based, personalized intervention that uses play-based techniques and positive reinforcement to help children develop essential skills, such as communication, social interaction, and daily living abilities. We deliver hands-on ABA therapy for children who learn differently, focusing on real progress through tailored plans led by our Board Certified Behavior Analysts (BCBAs) and supported by dedicated Registered Behavior Technicians (RBTs). This approach not only builds skills but also fosters real connections between children and their families, all while aligning with Individualized Education Programs (IEPs) for school-aged kids.
Medicaid benefits for ABA services typically include assessments, one-on-one sessions, and parent coaching, with 48 states currently offering coverage as per recent federal data from Medicaid Autism Services. At Heart Core ABA, we specialize in verifying benefits, coordinating prior authorizations, and providing in-home, school-based, or center-based services across Missouri and nearby Illinois. For instance, we recently helped a Springfield family navigate their Medicaid approval, ensuring seamless access to weekly sessions without upfront costs–though we always recommend verifying coverage, as prior authorization may be required and results may vary.
Understanding these fundamentals is the first step. In the sections ahead, we’ll explore ABA therapy Medicaid eligibility basics, like needing an autism diagnosis and being under 21, along with application processes and potential costs to help you access ABA through Medicaid effectively.
Fundamentals of ABA Therapy and Medicaid Coverage
At Heart Core ABA, we see how foundational knowledge empowers families navigating autism support. Applied Behavior Analysis, or ABA therapy, uses evidence-based techniques to help children who learn differently build essential skills. Core principles like positive reinforcement encourage positive behaviors while reducing challenges, focusing on areas such as social interactions, communication, and daily living routines. Imagine a child learning to greet a friend through playful, guided practice – that’s the real progress we foster with hands-on ABA therapy for children who learn differently.
Medicaid plays a vital role as a funding source for behavioral health services, especially for low-income families seeking quality care. Does medicaid cover aba therapy? Yes, through federal guidelines, it often does when deemed medically necessary, opening doors to accessible interventions like ABA Therapy Medicaid. We specialize in verifying insurance benefits and coordinating prior authorizations to ensure families in Missouri and Illinois communities receive the support they need without unnecessary barriers.
A key framework is the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit under Medicaid, which mandates coverage of necessary services for children under 21. This federal provision ensures that kids with autism spectrum disorder get comprehensive care, including behavioral therapies, as long as they’re restorative or preventive. As per federal guidelines from the Medicaid Autism Services resource, EPSDT requires states to provide these benefits without arbitrary limits, promoting equitable access across the country.
The following table outlines the basics of federal versus state approaches to ABA coverage:
| Aspect | Federal Guidelines (EPSDT) | State Variations (Examples) |
|---|---|---|
| Coverage Mandate | Requires coverage if medically necessary | Varies; some states limit hours |
| Eligible Services | Assessments, 1:1 therapy, parent training | Often includes in-home and school-based |
States implement EPSDT differently due to local policies and budgets, leading to variations in hours or settings. For instance, while federal rules set a baseline, some states cap weekly sessions at 20-40 hours, addressing questions like how much ABA therapy Medicaid pays for. Families can explore state resources through official Medicaid websites for precise details on aba therapy medicaid eligibility in their area, and we’re here to guide you through Missouri and Illinois specifics.
Medicaid aba therapy coverage typically includes key components like BCBA assessments to create personalized therapy plans, RBT-led 1:1 sessions for targeted skill-building, and family training to empower parents at home. These Medicaid-funded ABA interventions often cover in-home or school-based services, aligning with IEPs for seamless support. At Heart Core ABA, our BCBA supervision ensures consistent, care that comes straight from the heart, with weekly updates to track real connection and growth. Note that prior authorization may be required, and results may vary – always verify coverage with your provider.
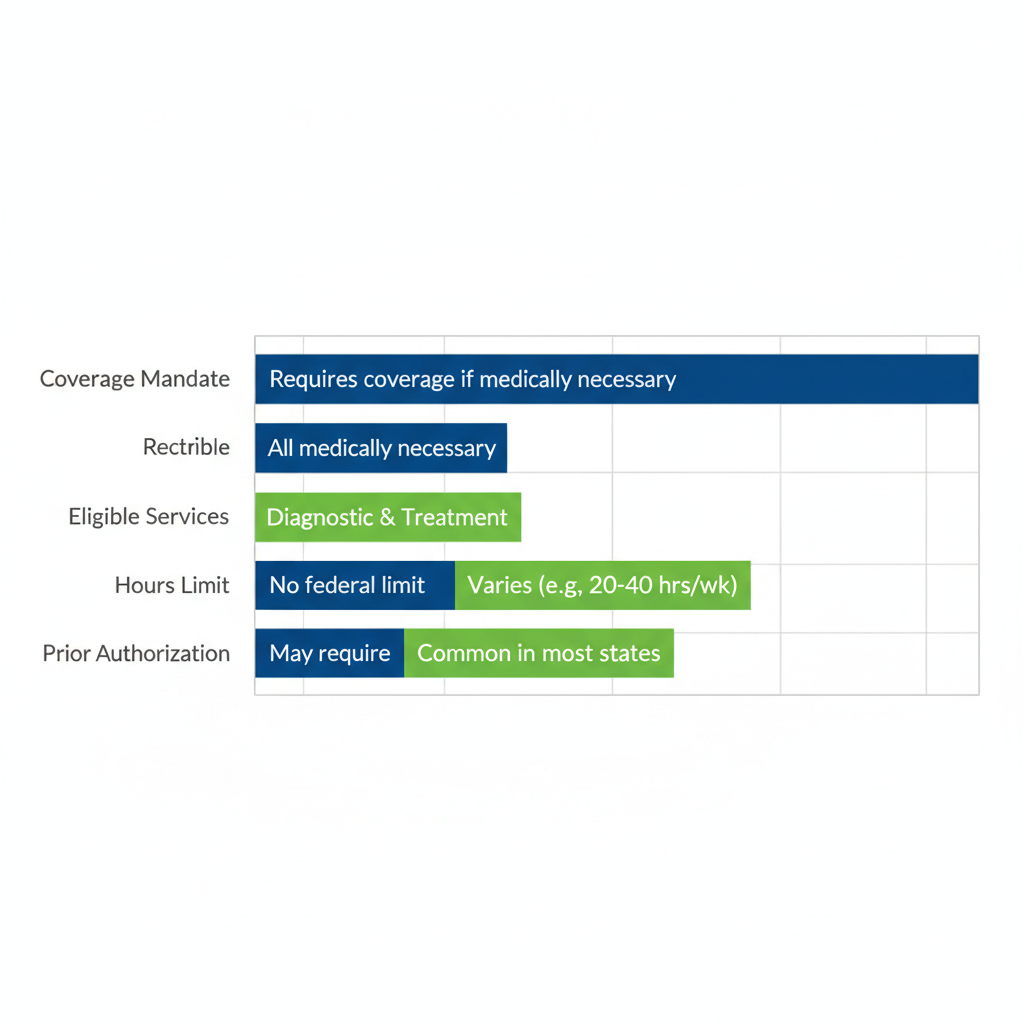
Federal vs. state Medicaid ABA therapy coverage comparison chart
This foundational overview shows how state ABA benefits under Medicaid provide a pathway to essential services, though details like exact hours depend on location. As we transition to deeper eligibility discussions, understanding these basics helps families advocate effectively for their child’s needs.
Deep Dive into Eligibility and Requirements
Navigating eligibility for ABA therapy under Medicaid can feel overwhelming, but we at Heart Core ABA are here to guide families through it. With our experience helping children in Missouri and Illinois access care, we break down the key factors like diagnosis, age, and income that determine if your child qualifies for these vital services. Understanding these requirements empowers you to take the next steps confidently.
Who Qualifies for Medicaid ABA Coverage
Qualifying for Medicaid ABA benefits starts with a formal diagnosis of autism spectrum disorder from a qualified professional, such as a licensed psychologist or developmental pediatrician. We often see families in our practice needing this documentation to initiate the process, as it confirms the medical necessity of ABA therapy. Age plays a crucial role too; Medicaid typically covers children under 21, aligning with federal guidelines to support early intervention where it matters most.
Income factors are central to aba therapy medicaid eligibility, as Medicaid is designed for low-income families meeting state-specific thresholds based on the federal poverty level. For instance, households at or below 138% of that level in expansion states may qualify, but exact figures vary. Does medicaid cover aba therapy? It does for those who meet these criteria, though prior authorization is often required to verify medical need. We recommend gathering school records or evaluations early to strengthen your application. Common documents include Individualized Education Programs (IEPs), medical assessments, and proof of residency. This thorough approach helps ensure smooth access to personalized therapy plans that drive real progress.
The following table outlines the consistency in core eligibility criteria while highlighting nuances:
| Criteria | Federal EPSDT | Missouri Example | Illinois Example |
|---|---|---|---|
| Diagnosis Required | Autism spectrum disorder via qualified provider | Same, with state assessment | State-licensed eval |
| Age Limit | Under 21 for full benefits | Up to 21 | Birth to 21 |
These alignments stem from federal standards, yet states add layers like assessment protocols. To navigate documentation, we advise organizing IEPs, diagnostic reports, and income verification upfront. Consult your state’s Medicaid office for personalized guidance, as requirements evolve.
Role of EPSDT in ABA Access
The Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) provision is a cornerstone of medicaid aba therapy coverage for children. As outlined in official Medicaid guidelines, EPSDT requires states to provide all medically necessary services to eligible kids under 21, even if not typically covered under standard plans. This ensures comprehensive ABA entitlements, covering assessments, therapy sessions, and parent training without arbitrary limits.
We have witnessed EPSDT-driven ABA access transform lives, like when a Missouri family secured intensive hours for their toddler after screening revealed needs. It mandates periodic check-ups to identify developmental delays early, making ABA a covered benefit when recommended. Remember, results may vary, and verifying coverage is essential. This framework promotes equity, helping families like yours build real connections through hands-on care.
State-Specific ABA Medicaid Rules
While federal guidelines set the foundation, state-specific ABA Medicaid rules create important variations that affect access. In the Midwest, for example, Missouri emphasizes provider networks and prior authorizations, often capping initial hours while requiring ongoing progress reports. Illinois, leveraging its Medicaid expansion, offers broader EPSDT implementation but may involve stricter evaluation processes through state-licensed professionals.
These differences mean eligibility in Missouri might hinge on coordination with local agencies, whereas rules in Illinois focus on integrating ABA with school-based IEPs. For instance, both states cover aba therapy covered by medicaid for diagnosed children under 21, but Missouri limits adult services, and Illinois prioritizes early intervention for toddlers. Income thresholds also differ; Missouri allows up to 300% of the federal poverty level for kids, providing more flexibility than some regions.
The table below compares these elements to illustrate the landscape:
| Aspect | In-Home Therapy | Center-Based Therapy |
|---|---|---|
| Coverage Availability | Typically covered if prescribed | Often requires facility approval |
| Cost Expectations | Low copays | Potential session limits |
This comparison highlights how federal EPSDT ensures a baseline, but state interpretations add practical hurdles like hour caps or network requirements. We guide families through these, from insurance verification to appeals, but always advise checking your state Medicaid website for the latest details. Prior authorization may be required, and consulting a healthcare professional helps tailor applications. Our BCBA-led teams in Missouri and Illinois specialize in IEP coordination, ensuring care aligns with these rules for measurable skill development.
Practical Steps for Applying for Medicaid ABA Coverage
Applying for Medicaid coverage for ABA therapy can feel overwhelming, but we’re here at Heart Core ABA to guide you through it with practical steps tailored for families in Missouri and Illinois. Many parents wonder, does medicaid cover aba therapy? The answer is yes in most cases for eligible children with autism spectrum disorder, but it requires careful navigation of the process. We’ll break it down into clear actions, from gathering documents to selecting providers, ensuring you understand how to access these vital services that support real progress and real connection in your child’s development.
Gathering Documentation and Initial Steps
Starting the journey for ABA Therapy Covered By Medicaid begins with confirming aba therapy medicaid eligibility and collecting the right paperwork. You’ll need a formal diagnosis of autism from a qualified healthcare professional, such as a psychologist or pediatrician, along with any Individualized Education Program (IEP) if your child is school-aged. Income verification forms, like recent pay stubs or tax returns, are essential to prove household eligibility, and don’t forget proof of residency in Missouri or Illinois. Under the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefits, Medicaid must cover necessary services for children under 21, so include any evaluation reports that outline your child’s behavioral needs.
To get started, contact your local Medicaid office or visit the state portal–Missouri’s MO HealthNet or Illinois’ Medical Assistance site–to begin enrollment. We recommend creating a checklist: 1) Schedule a diagnostic assessment if needed; 2) Gather financial documents; 3) Complete the application form online or in person; 4) Submit everything within the 30-day processing window. This initial phase typically takes 30 to 90 days for approval, but acting promptly helps avoid delays. At Heart Core ABA, we assist families with this paperwork to make applying for ABA Medicaid benefits smoother, always reminding you to verify details with your state’s guidelines.
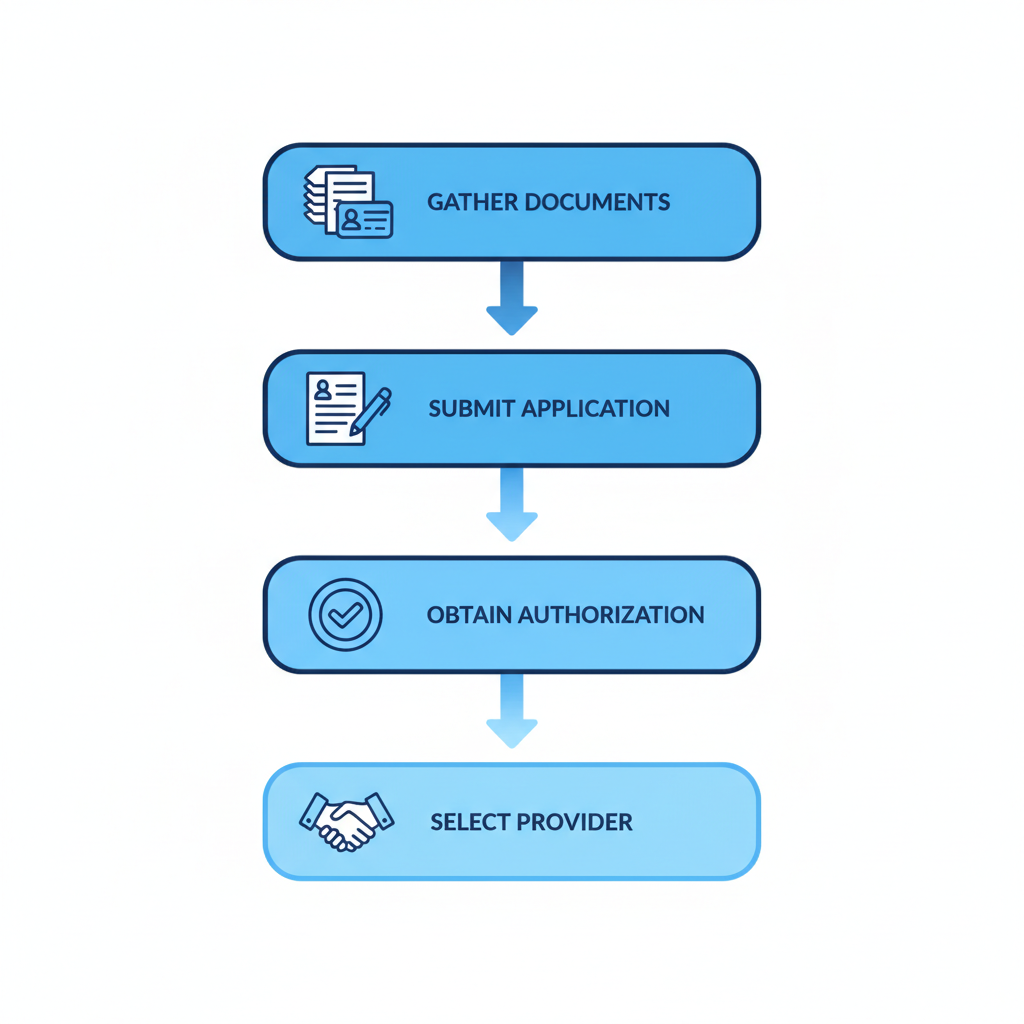
Steps to apply for Medicaid coverage of ABA therapy services
These steps form the foundation for accessing hands-on ABA therapy for children who learn differently, and following them ensures you’re prepared for the next phases.
Navigating Authorization and Provider Selection
Once enrolled, focus on the prior authorization process for medicaid aba therapy coverage, which involves a Board Certified Behavior Analyst (BCBA) conducting an initial assessment to determine therapy needs. Submit this functional behavior assessment, along with your child’s treatment plan, to Medicaid for review–states must cover prescribed ABA services as outlined in federal guidelines. Expect a decision within 14 to 45 days; if approved, you’ll receive details on covered hours, often up to 40 weekly for intensive programs.
Choosing the right provider is key–opt for in-network options like Heart Core ABA to minimize out-of-pocket costs and streamline billing. We verify benefits upfront and handle authorizations, coordinating with your IEP for school-based integration. Look for providers offering personalized therapy plans with BCBA supervision and RBT-delivered 1:1 sessions. In Missouri and Illinois, prioritize those experienced in Medicaid approval for therapy, ensuring seamless care that comes straight from the heart. Remember, prior authorization may be required, so consult your plan for specifics.
In-Home vs. Center-Based Coverage Under Medicaid
When deciding on delivery models, in-home ABA therapy offers flexibility right in your living space, ideal for building routines in familiar environments, while center-based programs provide structured social opportunities in a dedicated facility. Both models support measurable skill development through play-based methods, aligning with family collaboration and weekly parent updates at providers like ours.
The following table outlines key differences in Medicaid coverage for these settings in Missouri and Illinois:
| Cost Element | Typical Medicaid Coverage | Potential Family Costs |
|---|---|---|
| Copays | Covered services often $0-$3/session | Income-based |
| Annual Limits | EPSDT no cap if necessary | Out-of-pocket max applies |
Medicaid generally includes both under EPSDT for prescribed services, with in-home emphasizing personalized 1:1 instruction and center-based allowing peer interactions in small social skills groups. As outlined in Medicaid Autism Services guidelines, states must cover these if medically necessary, though facility approvals can add steps for centers.
At Heart Core ABA, we support both in-home and center-based options, verifying coverage and tailoring plans to your family’s needs–whether it’s early intervention for toddlers at home or structured sessions in our centers. This flexibility ensures care that fits your lifestyle while focusing on real progress.
Navigating these steps empowers you to secure the support your child deserves, and we’re ready to partner with you every step of the way.
Advanced Considerations for Medicaid ABA Coverage
At Heart Core ABA, we understand the complexities that come with advanced Medicaid ABA planning, especially when families in Missouri and Illinois navigate beyond-basics coverage considerations. Drawing from our experience coordinating insurance benefits, including hands-on ABA therapy for children who learn differently, we help families anticipate potential challenges like costs, age limits, and eligibility nuances. Our team verifies insurance and assists with prior authorizations to make real progress toward real connection and care that comes straight from the heart.
When families ask, “does medicaid cover aba therapy,” cost expectations often top their concerns. Under Medicaid, aba therapy medicaid typically covers core services like 1:1 sessions and social skills groups with minimal out-of-pocket expenses for eligible children. Copays are often low or waived, ranging from $0 to $3 per session depending on family income. Deductibles are rare for behavioral therapies, but an annual out-of-pocket maximum may apply after other medical costs. For instance, imagine a family in Missouri starting weekly sessions; they might face just a small copay if their income qualifies for reductions.
Costs vary widely due to state-specific rules in Missouri and Illinois, family income levels, and the scope of services needed. The Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit under Medicaid mandates coverage for necessary services without caps if they’re deemed essential for a child’s development, overriding typical state limits. This ensures personalized therapy plans, like our in-home ABA therapy or school-based services, remain accessible.
This table highlights key cost factors in Medicaid ABA therapy. To plan effectively, we recommend tracking household income annually and appealing denials promptly–EPSDT provides strong grounds for necessary extensions. Budget by setting aside a small fund for copays and consulting our insurance navigation team for verification; prior authorization may be required, and results may vary.
Turning to age-related questions, medicaid aba therapy coverage for adults is limited, as most states cap eligibility at age 21. In Missouri and Illinois, ABA services focus on children and teens, rarely extending post-21 unless tied to ongoing EPSDT needs during transitions. However, extensions are possible through appeals if therapy supports independence. Social skills groups, a core offering at Heart Core ABA, often fall under this coverage for school-aged kids, helping build real connections in small, play-based settings.
Income plays a key role in aba therapy medicaid eligibility, requiring verification of household earnings to determine if your child qualifies under parental or guardian benefits. For families in Illinois, even moderate incomes rarely disqualify kids from essential services, thanks to EPSDT protections. We see waiting lists in high-demand areas, but appeals can expedite access–always document medical necessity. Hypothetically, a family facing income changes might reapply seamlessly with our caregiver coaching support. Remember to verify insurance coverage, as it’s not a substitute for professional medical advice.
Frequently Asked Questions on Medicaid ABA Coverage
Does Medicaid cover ABA therapy? Yes, under the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit, Medicaid often covers ABA therapy for eligible children with autism, though details vary by state. We can verify your aba therapy covered by insurance benefits at Heart Core ABA.
How does medicaid aba therapy coverage differ by state? Coverage levels depend on state Medicaid plans; some fully fund it via waivers, others limit sessions. Check your state’s Medicaid site or contact us for Missouri and Illinois specifics, as referenced in federal autism services guidelines.
What determines aba therapy medicaid eligibility? Eligibility typically requires a diagnosis of autism spectrum disorder in children under 21, plus medical necessity documentation. Results may vary, so consult your provider and verify with us.
What tips help with Medicaid ABA applications? Gather medical records, complete prior authorizations promptly, and appeal denials if needed. Our team assists with paperwork for smoother access in Missouri or Illinois.
Are there costs with Medicaid ABA? Most plans cover comprehensively, but small co-pays or deductibles may apply. Prior authorization is often required; we handle verification to minimize surprises.
Does Medicaid cover in-home ABA therapy? Yes, many states approve in-home services for convenience. We deliver personalized plans in-home across Missouri and nearby Illinois to support real progress.
Next Steps in Accessing Medicaid for ABA Therapy
In summary, yes, does medicaid cover aba therapy for eligible children with autism in Missouri and Illinois through robust medicaid aba therapy coverage. Understanding aba therapy medicaid eligibility starts with verifying your child’s diagnosis and applying via state portals–it’s straightforward and often cost-free under EPSDT protections that federal rules ensure access to necessary treatments.
At Heart Core ABA, we’re here to guide your Medicaid ABA journey with personalized support in Missouri and Illinois, from insurance verification to hands-on ABA therapy delivery. Reach out to us today for tailored advice and take the first step toward real progress and connection for your family.















