ABA Therapy Medicaid
Table of Contents
Navigating ABA Therapy Coverage Under Medicaid
Navigating ABA therapy Medicaid coverage can feel overwhelming for families supporting children with autism. We at Heart Core ABA understand the complexities of securing state-sponsored autism therapy, especially when asking, ” does medicaid cover aba therapy?” The good news is that Medicaid often funds these essential interventions, helping families access hands-on ABA therapy for children who learn differently.
Applied Behavior Analysis, or ABA, is a structured intervention designed to build vital skills like communication and social interaction in children with autism. Under Medicaid’s Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefits, all states must provide ABA under EPSDT for eligible children, as outlined in federal guidelines. In Missouri and Illinois, coverage includes in-home and school-based Medicaid-funded ABA interventions through local ABA Therapy Covered By Medicaid. At Heart Core ABA, our team of credentialed Board Certified Behavior Analysts and Registered Behavior Technicians verifies benefits, coordinates prior authorizations, and offers services like parent coaching and social skills groups. We focus on real progress through personalized therapy plans, with weekly updates to ease family stress. Remember, prior authorization may be required, and we encourage verifying coverage with your provider.
This guide will explore eligibility criteria, detailed benefits, the step-by-step process, and best practices for finding aba therapy medicaid providers near me in Missouri and Illinois, empowering you to take confident next steps toward care that comes straight from the heart.
Understanding Medicaid Eligibility for ABA Therapy
At Heart Core ABA, we understand how crucial it is for families to access Does Medicaid Cover ABA Therapy when seeking support for children with autism. Navigating eligibility can feel overwhelming, but we’re here to guide you through the process, ensuring you have the information needed to unlock hands-on ABA therapy for children who learn differently. This section breaks down the key requirements, focusing on Missouri and Illinois, where our services make real progress through real connection and care that comes straight from the heart.
Eligibility Criteria in Missouri and Illinois
Qualifying for ABA therapy Medicaid starts with a formal diagnosis of autism spectrum disorder, typically established through DSM-5 criteria by a qualified healthcare professional. In Missouri and Illinois, children must meet income-based Medicaid thresholds, often covering families up to 300% of the federal poverty level, aligning with the federal Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) mandate that requires states to provide ABA as a necessary service. We see many families qualify if their child is under 21, with early intervention programs available from as young as 18 months for toddlers showing developmental delays.
For school-aged children, coordination with an Individualized Education Program (IEP) can strengthen eligibility, especially when functional assessments reveal skill deficits in communication or social interaction. In Missouri’s MO HealthNet program, autism-specific expansions ensure coverage for intensive behavioral interventions, while Illinois Medicaid emphasizes comprehensive autism waivers for broader access. Does medicaid cover aba therapy? Yes, in these states, it often does for diagnosed children meeting these criteria. Our team helps verify eligibility, assisting with the steps to confirm your child’s access to personalized therapy plans.
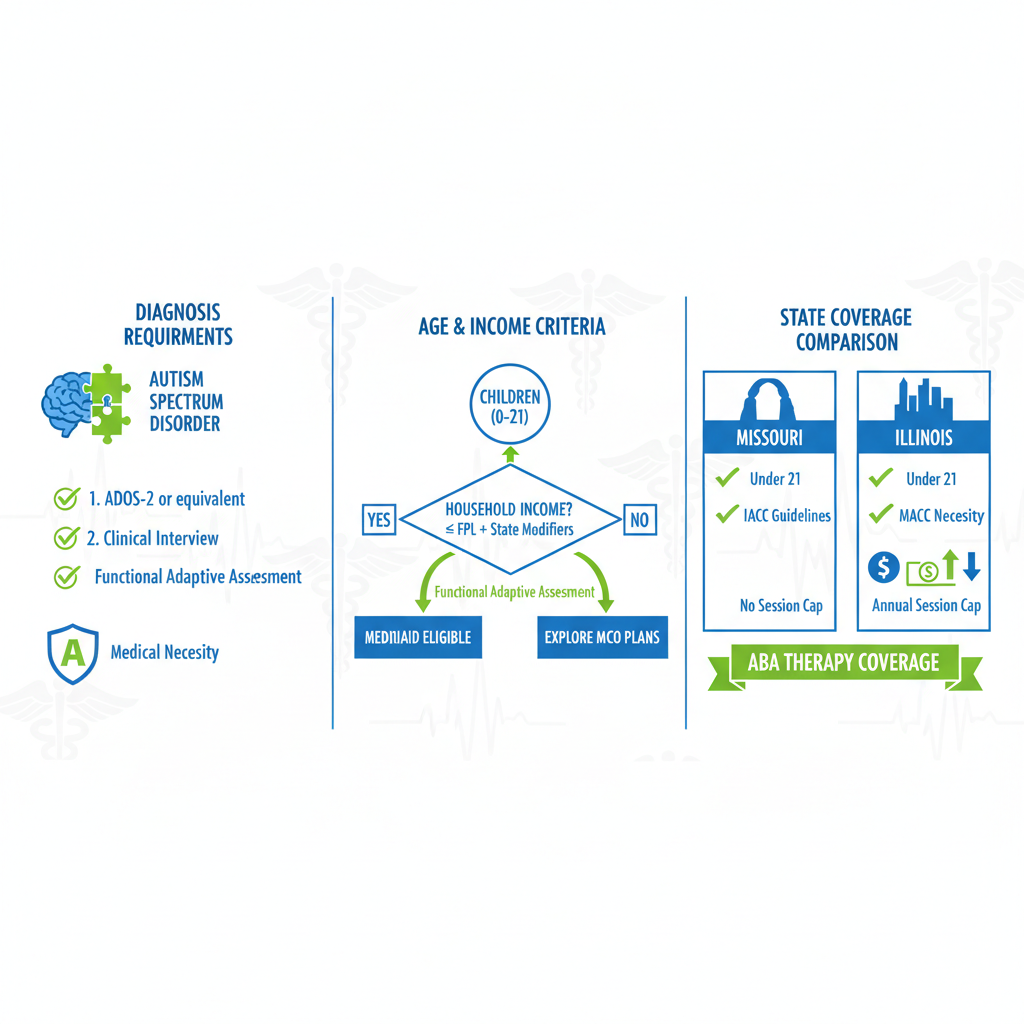
Medicaid eligibility overview for ABA therapy services in Missouri and Illinois
This visual highlights how straightforward the process can be once you understand the basics, allowing families to focus on progress rather than paperwork.
Documentation and Application Basics
Applying for Medicaid eligibility for autism interventions requires gathering key paperwork to demonstrate need. Start with a medical diagnosis from a licensed physician or psychologist, confirmed via standardized tools like the ADOS-2 for autism. Functional assessments, such as the VB-MAPP, evaluate your child’s current abilities and pinpoint areas for ABA support, like daily living skills or behavior management.
Income verification through pay stubs or tax returns proves financial eligibility, while a referral from a primary care provider often initiates the process. In both Missouri and Illinois, applications go through state portals, with approvals typically within 45 days per recent Medicaid SPA 2024 updates on autism benefits. We assist families by compiling these documents, coordinating prior authorizations, and even connecting you with aba therapy medicaid providers near me in Springfield, Illinois, or St. Louis, Missouri.
For example, one family we supported submitted their child’s IEP alongside the diagnosis, streamlining approval for in-home sessions. Remember, prior authorization may be required, and we recommend verifying insurance coverage with your plan. Our insurance verification services take the burden off your shoulders, fostering real connection as you begin this journey.
Variations Across States
While federal guidelines set the foundation for state-funded ABA access, Missouri and Illinois implement them with unique twists to better serve local families. Missouri’s MO HealthNet fully embraces EPSDT, covering up to 40 hours weekly of ABA for eligible children, with high state compliance rates noted in federal Medicaid Autism Services reports–over 95% for core benefits. Illinois, through its autism mandate, offers enhanced waivers that include parent coaching and social skills groups, sometimes extending coverage beyond standard limits for severe cases.
These differences stem from state-specific expansions; for instance, Illinois prioritizes community-based integration, while Missouri focuses on rural access via telehealth options. Both states align with national standards, but approval timelines vary–Missouri processes faster for toddlers at 18 months, per SPA 2024 policy shifts. At Heart Core ABA, we tailor our BCBA assessments and RBT-delivered 1:1 therapy to these variations, ensuring IEP coordination fits seamlessly.
A family in Illinois recently benefited from our school-based ABA therapy under Medicaid, gaining extended hours not always available in other states. Results may vary, so consult a healthcare professional for personalized advice. We’re committed to helping you navigate these nuances for the best outcomes.
Benefits of Medicaid-Funded ABA Therapy
At Heart Core ABA, we see families thrive when they access ABA therapy Medicaid options. These programs offer real progress in skill development and provide essential financial support, making personalized interventions accessible for children with autism in Missouri and Illinois. By leveraging Medicaid-funded services, parents gain peace of mind knowing their child’s growth is prioritized without overwhelming costs.
Skill Development and Family Support
Medicaid-funded ABA therapy empowers children to build vital skills through targeted, play-based sessions. We focus on communication, social interactions, and daily living abilities, helping kids navigate their world more independently.
Evidence from the CDC highlights ABA’s effectiveness, with studies showing up to 47% gains in key skills like language and self-care. For instance, our 1:1 sessions with Registered Behavior Technicians (RBTs) under BCBA supervision break down complex tasks into manageable steps, fostering confidence and reducing challenging behaviors. Parent coaching is a cornerstone, teaching families techniques to reinforce learning at home, which extends therapy’s impact beyond clinic walls.
- Improved verbal expression during playtime
- Better turn-taking in family routines
- Enhanced emotional regulation for smoother transitions
We integrate this family training seamlessly, providing weekly updates to ensure collaborative progress and lasting connections.
Cost Coverage and Session Limits
One of the biggest advantages of Medicaid-supported behavior interventions is the comprehensive cost coverage it provides. Families often wonder, does medicaid cover aba therapy, and the answer is yes for eligible children, typically with $0 copay requirements.
Medicaid reimbursement rates in Missouri and Illinois support up to 40 hours per week based on individual needs and prior authorization, as outlined in state autism services guidelines. This funding covers assessments, ongoing therapy, and progress monitoring without out-of-pocket expenses for approved plans. Coverage duration ties to the child’s development milestones, often extending through school years as long as benefits are demonstrated, allowing sustained intervention without abrupt interruptions.
At Heart Core ABA, our team handles insurance verification and billing, easing the administrative burden so families can focus on their child’s journey. This affordable autism therapy program ensures equitable access, aligning with IEP goals for holistic support.
Access to Diverse Service Options
Medicaid opens doors to flexible service delivery, including in-home, school-based, and group settings tailored to each family’s lifestyle. This variety ensures therapy fits seamlessly into daily routines, promoting consistent engagement.
Our programs emphasize hands-on ABA therapy for children who learn differently, with options like in-home visits for comfort or school collaborations for real-world practice. Social skills groups encourage peer interactions, vital for building friendships and empathy. Drawing from Medicaid Autism Services data, states approve diverse formats to meet unique needs, such as early intervention for toddlers or center-based sessions for structured learning.
When searching for aba therapy medicaid providers near me, families in the Kansas City or St. Louis areas find our BCBA-led teams offering consistent RBT matches for trust and rapport. We coordinate with schools for IEP alignment, delivering care that comes straight from the heart and supports real connection through personalized therapy plans.
How ABA Therapy Works with Medicaid
At Heart Core ABA, we make ABA therapy Medicaid accessible by guiding families through the processes that ensure real progress and real connection. Understanding how aba therapy covered by medicaid works helps families in Missouri and Illinois communities access hands-on ABA therapy for children who learn differently. We streamline this for you, focusing on personalized therapy plans that align with funded behavior analysis processes.
Prior Authorization Process
Securing prior authorization is a key step when families ask, “does medicaid cover aba therapy?” We start by conducting a comprehensive BCBA assessment to evaluate your child’s needs, drawing from Medicaid guidelines like those in state plan amendments that require detailed documentation for approval. This assessment identifies target behaviors and skill gaps, forming the foundation for eligibility.
- Initial Evaluation: Our Board Certified Behavior Analyst (BCBA) completes a functional behavior assessment within the first two weeks, gathering input from parents and educators.
- Treatment Plan Development: Based on the evaluation, we create a customized plan outlining goals, interventions, and progress measures, typically ready in 7-10 days.
- Submission to Medicaid: We submit the plan along with required docs, such as diagnosis confirmation and medical necessity letters, to your state’s Medicaid office–expect a 30-60 day review timeline, adapted from models like Utah’s ASD programs but tailored for Missouri and Illinois.
- Approval and Updates: Once approved, we provide weekly updates to track adjustments, ensuring compliance with Medicaid-approved treatment protocols.
These steps emphasize teamwork, with our expertise handling paperwork to reduce family stress. Remember, prior authorization may be required, and we recommend verifying coverage early.
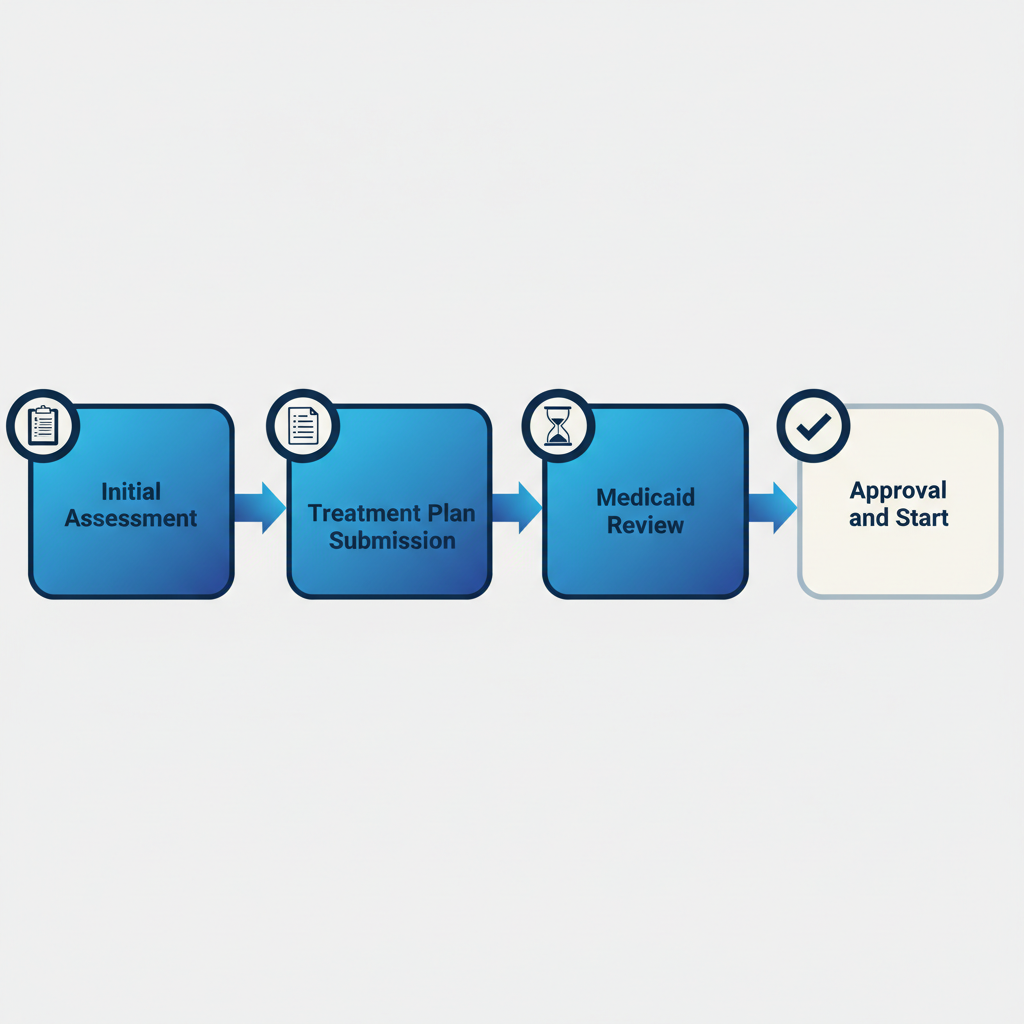
Medicaid prior authorization steps for ABA therapy services
This visual outlines the journey clearly, helping families visualize the path to starting services. Building on approval, we integrate family input to refine plans for better outcomes.
Service Delivery and Coordination
Once authorized, ABA therapy Medicaid providers near me deliver sessions through coordinated, flexible scheduling that fits your family’s life in Illinois or across Missouri communities. Our RBTs provide 1:1 therapy in settings like in-home ABA therapy, center-based programs, or school-based services, all under BCBA supervision for consistent care that comes straight from the heart.
Sessions typically last 2-4 hours, 3-5 days a week, with data tracking via digital tools to monitor progress in real-time. We coordinate with schools for IEP integration, ensuring school-based ABA therapy aligns with educational goals without disrupting routines. Billing occurs monthly, with copay exemptions often applying for qualifying families, and we handle claims to keep things seamless.
Tips for smooth coordination: Communicate preferred times early, attend family training sessions for at-home reinforcement, and use our weekly parent updates to stay involved. If delays occur, private-pay bridges can maintain momentum while awaiting full funding. This approach fosters real connection and measurable skill growth.
Insurance Verification Steps
We assist with insurance verification to confirm benefits and answer questions like, “How do I qualify for ABA therapy under Medicaid?” Our team starts by reviewing your Medicaid card and diagnosis details to verify eligibility for services such as early intervention for toddlers or social skills groups.
- Benefit Confirmation: Contact your state Medicaid office with us to check coverage limits, like hours per week or age caps, using resources modeled on established ASD family assistance programs.
- Documentation Gathering: Collect necessary forms, including proof of autism diagnosis and prior auth if needed–we guide you through this to avoid denials.
- Claims Handling: Post-approval, we submit claims electronically, tracking payments and appealing any issues, with billing cycles aligned to your plan.
- Ongoing Support: Provide updates on any changes, like rate adjustments from state plans, ensuring uninterrupted access.
Our insurance verification and Medicaid assistance lighten the load, but always consult a healthcare professional for personalized advice. Results may vary, and information here isn’t a substitute for professional medical guidance. This teamwork ensures families focus on progress.
Best Practices for Accessing Medicaid ABA Therapy
Navigating aba therapy medicaid can feel overwhelming for families, but with the right steps, you can connect your child with effective support. At Heart Core ABA, we specialize in helping families in Missouri and Illinois access these vital services through our network of 42 BCBAs and 54 RBTs. We verify benefits, handle prior authorizations, and offer personalized plans that align with Medicaid coverage, ensuring real progress and connection for children on the autism spectrum.
Finding Reliable Providers
Start your search for ABA therapy Medicaid providers in Missouri or Illinois using official state directories, similar to Virginia’s DMAS Provider Finder. For Missouri, check the MO HealthNet portal; in Illinois, use the Health Care Services website to locate in-network options. We recommend searching for “aba therapy medicaid providers near me in Missouri” or adding your city like East St. Louis for targeted results. These tools list providers accepting Medicaid, helping you avoid out-of-pocket surprises.
For example, enter your zip code and filter for behavioral health services to find local options. Families often discover providers offering in-home or clinic-based therapy this way, streamlining the process. At Heart Core ABA, our team assists with these searches, coordinating everything from initial inquiries to enrollment.
Take action by calling state hotlines or visiting websites today–reach out to us for personalized guidance on finding matches in your area.
Choosing Between Service Settings
When deciding on settings, consider how each fits your child’s needs and routine, especially since does medicaid cover aba therapy in various environments like home, center, or school. Home-based offers flexibility for toddlers, allowing therapy in a familiar space with parent coaching integrated naturally. Center-based promotes socialization through small groups, while school options tie into IEPs for seamless support during the day.
In Missouri and Illinois, Medicaid-eligible autism providers often deliver all three, with home visits ideal for building daily skills and centers fostering peer interactions–our social skills groups exemplify this balance. School-based therapy coordinates with educators, reducing transitions and enhancing learning, as supported by CDC guidelines emphasizing family involvement for better outcomes.
Discuss options with providers; we at Heart Core ABA help evaluate what’s best, including private-pay bridges if coverage gaps arise, to keep therapy consistent.
Evaluating Provider Quality
Look for key indicators like BCBA-to-client ratios and family feedback when selecting local behavior therapy networks. Aim for providers with experienced teams–ours maintains consistent RBT matches for trust and progress. Check credentials via state boards and reviews on platforms like Google, focusing on consistency and parent satisfaction.
The CDC highlights that involving families in therapy boosts effectiveness, so prioritize services with regular updates and training. In areas like Missouri, seek Medicaid-eligible autism providers with high ratios, such as our 42 BCBAs supervising personalized plans. Read testimonials for real insights into outcomes and communication.
Schedule consultations to ask about supervision and customization; contact us to explore how our heart-centered approach ensures quality care tailored to your family.
Accessing ABA Therapy Medicaid for Your Family
Navigating aba therapy covered by insurance can open doors to essential support for your child’s autism journey. At Heart Core ABA, we see ABA therapy Medicaid as a vital resource that makes high-quality interventions accessible for families in Missouri and Illinois. Federal programs, like those outlined in Medicaid Autism Services, ensure broad access to these therapies, helping children build skills through evidence-based practices. If you’re wondering does medicaid cover aba therapy, the answer is yes for many eligible families, covering key elements like assessments and ongoing sessions.
Key takeaways include our family-centered approaches, such as parent coaching that empowers you to support your child’s growth at home. We prioritize early intervention to foster real progress and real connection, delivering hands-on ABA therapy for children who learn differently in in-home, school, or center settings. Our teams handle no-cost insurance verifications and coordinate with Medicaid to simplify the process, always with care that comes straight from the heart.
Ready to explore aba therapy medicaid providers near me? We’re here to partner with you in your Missouri or Illinois community for Medicaid-backed autism support and local therapy funding options. Contact us today for a personalized therapy plan, assessment, or answers to your questions–let’s take the next step toward your family’s brighter future. Remember to verify coverage, as prior authorization may be required.















