ABA Therapy Covered By Insurance
Table of Contents
Understanding ABA Therapy Insurance Coverage
At Heart Core ABA, we understand the challenges families face when seeking effective support for children with autism. ABA therapy, or Applied Behavior Analysis, is an evidence-based intervention that helps build essential skills like communication and social interaction through positive reinforcement. Knowing if aba therapy covered by insurance is crucial, as it can significantly reduce costs and make these vital services accessible for families across the US.
Thanks to advocacy efforts from organizations like Autism Speaks, over the past two decades, health insurance coverage for ABA has expanded dramatically, reaching at least 200 million people. Today, more than 95% of states have mandates requiring private insurers to cover ABA therapy for autism spectrum disorder, often up to age 21 or beyond. For families relying on public options, aba therapy medicaid coverage provides another lifeline, with many states offering comprehensive benefits through Medicaid waivers. However, common barriers such as prior authorizations can complicate access, requiring thorough documentation to prove medical necessity.
State variations mean that aba therapy insurance by state differs– for instance, a Missouri family might navigate specific requirements for in-home sessions, while those in Illinois benefit from robust school-based mandates. At Heart Core ABA, we specialize in verifying benefits, coordinating with insurers, and handling paperwork to streamline the process. Our team ensures personalized therapy plans align with your coverage, whether through private plans or state-mandated ABA benefits.
Understanding insurance for autism behavioral therapy is the first step toward real progress. As we explore further, you’ll learn practical tips for verification and overcoming hurdles. Remember, coverage details vary, so we recommend consulting your provider and verifying benefits–prior authorization may be required.
Basics of ABA Therapy Insurance
At Heart Core ABA, we often hear from families navigating the world of insurance for their child’s care. Understanding Autism Therapy Covered By Insurance starts with grasping how aba therapy covered by insurance works to support essential treatments like Applied Behavior Analysis (ABA). ABA therapy is a evidence-based approach focused on building skills for children with autism spectrum disorder (ASD), such as communication, social interaction, and daily routines. Early access to these autism behavioral therapy benefits can make a real difference, especially since ASD affects about one in 54 children according to the CDC. Yet, the costs–often $40,000 to $60,000 annually for intensive interventions–highlight why insurance coverage is crucial for families we serve in Missouri and Illinois.
To build a strong foundation, let’s define key terms that come up in insurance discussions for ABA:
- Prior Authorization: This is the insurer’s approval process before therapy begins, ensuring the treatment meets specific criteria.
- Medical Necessity: Coverage hinges on whether ABA is deemed essential for the child’s development, backed by professional assessments.
- EPSDT (Early and Periodic Screening, Diagnostic, and Treatment): A federal Medicaid program that covers comprehensive services for children under 21, including behavioral therapies when medically necessary.
These concepts, drawn from guidelines like those from Autism Speaks, help families prepare documentation such as a doctor’s diagnosis letter and behavioral assessments. We at Heart Core ABA guide families through this, emphasizing that a formal ASD diagnosis is typically the first step for approval.
Federal influences, like the Affordable Care Act (ACA), set the stage by requiring essential health benefits, which indirectly support autism treatments. However, the real action happens at the state level with autism mandates. According to the National Conference of State Legislatures (NCSL), all 50 states now require private insurers to cover ABA therapy under state autism insurance requirements, though details vary. This means aba therapy insurance by state can differ in scope, age limits (often up to 21), and benefit caps. For instance, in Missouri, mandates ensure coverage for medically necessary services, aligning with our hands-on ABA therapy for children who learn differently. These laws aim to ease the financial burden, but families should verify specifics, as prior authorization may be required.
When exploring insurance options, families often compare private plans and public programs like Medicaid. Private insurance, typically through employers or marketplaces, follows state mandates more uniformly.
| Aspect | Private Insurance | Medicaid |
|---|---|---|
| Coverage Mandate | Required in 50 states via autism mandates | Varies by state; federal EPSDT for children |
| Typical Session Limit | 20-40 hours/week, up to age 21 | State-dependent; often unlimited for medically necessary |
This overview, informed by NCSL state laws and Medicaid.gov guidelines, shows how private insurance provides structured access but may include caps, while Medicaid prioritizes necessity without strict hour limits in many cases. For example, private plans might cover 80-100% after deductibles, but session totals could hit annual benchmarks. Medicaid, on the other hand, often extends broader support for low-income families, making aba therapy medicaid coverage a vital lifeline. At Heart Core ABA, we handle verification to clarify these differences, ensuring real progress through personalized therapy plans.
Building on this comparison, private insurance frequently covers a higher percentage of costs post-approval–Autism Speaks notes about 90% of plans do so once authorized–but documentation like progress reports is key to maintaining benefits. Public options like Medicaid emphasize ongoing medical necessity, which can mean fewer upfront barriers for eligible children. Typical coverage ranges from 80% to full reimbursement, depending on the plan and state, though out-of-pocket elements like copays apply. We see families succeed when they start with a clear diagnosis and assessment, as this directly answers what documentation insurance needs for ABA approval.
In our experience, understanding how much insurance typically pays–often the bulk after meeting deductibles–empowers families to focus on care. As we transition to deeper state variations, keep in mind that while federal frameworks provide a baseline, checking local rules in Missouri or Illinois ensures the best fit. Remember, results may vary, and it’s wise to consult professionals for personalized advice on coverage.

Comparison of private vs. public insurance for ABA therapy coverage
This visual reinforces the trade-offs, where private plans offer predictability and Medicaid flexibility. For families we support, combining this knowledge with our insurance navigation services–like coordinating prior authorizations–fosters care that comes straight from the heart, leading to real connection and growth.
State-Specific ABA Therapy Mandates
Understanding how ABA therapy insurance varies across the US can feel overwhelming, but we are here to break it down for families navigating these rules. With nearly every state addressing coverage for autism treatments, regional differences play a big role in access to essential services like ABA. These mandates stem from a mix of federal guidelines under the Affordable Care Act, which encourages essential health benefits including behavioral therapies, and state-level laws that fill in the details.
Overview of National Coverage Trends
Since the early 2000s, autism awareness has grown, leading to widespread legislative action. Today, 47 states require some form of private insurance coverage for autism-related treatments, including ABA therapy covered by insurance. This trend reflects a national push for equity, as highlighted in the 2022 IACC Report to Congress, which notes rising access since 2010 through expanded mandates and public programs. Federal influences like the ACA have set a foundation by classifying preventive screenings and early interventions as essential, prompting states to align their policies. Overall compliance shows steady progress, with most states mandating coverage up to age 21, though caps and exceptions vary widely.
The following table illustrates national versus regional trends in these mandates, drawing from NCSL data on state laws.
| State | Mandate Year | Age Limit | Annual Cap |
|---|---|---|---|
| Missouri | 2010 | 21 | $50,000 |
| Illinois | 2008 | 21 | No cap |
This comparison underscores how the vast majority of states have stepped up with requirements, but the three without private mandates often rely on federal options like Medicaid for support. Such trends mean families in mandated states enjoy more predictable access, while others may face hurdles that require creative navigation.
Key State Variations and Mandates
State laws on aba therapy insurance by state reveal fascinating differences in scope and stringency. For instance, Missouri’s 2010 mandate, informed by NCSL summaries, requires coverage for children up to age 21 but includes a $50,000 annual cap, balancing insurer costs with family needs. This cap can limit intensive ABA sessions, which research shows often cost $40,000 to $60,000 yearly per child. In contrast, Illinois adopted its law in 2008, offering broader protection with no dollar caps and coverage extending to age 21, making it easier for families in Illinois communities to access ongoing aba therapy insurance by state without financial ceilings.
These examples highlight regional autism therapy mandates at work. California, another leader since 2012, also provides uncapped coverage up to age 21, emphasizing comprehensive state-specific behavioral benefits. Enforcement falls to state insurance departments, which oversee compliance and handle appeals, ensuring plans adhere to these rules. However, self-insured employer plans may qualify for exemptions, adding a layer of complexity that families must check.
To further illustrate these variations, consider the table below based on state insurance department summaries and NCSL data:
| Step | Private Insurance | Medicaid |
|---|---|---|
| Initial Contact | Call member services; 1-2 days | Contact state agency; 5-10 days |
| Documentation Submission | Diagnosis, assessment; 2-4 weeks approval | EPSDT screening; 30-90 days |
Missouri’s approach offers solid but bounded support, ideal for moderate needs, while Illinois and California prioritize unrestricted access, potentially covering more hours of therapy. We help families in Missouri and nearby Illinois communities decode these rules, verifying benefits to maximize what’s available under local laws. This patchwork encourages families to research state-specific details early.
Implications for Families Seeking Coverage
These state-specific ABA Therapy Mandates directly impact how easily families can secure care, with stronger laws reducing out-of-pocket burdens and improving outcomes for children on the spectrum. In mandate-heavy states like Illinois, access feels more seamless, but even capped policies in Missouri provide a vital safety net compared to non-mandated areas. For families in states with limited requirements, turning to aba therapy medicaid coverage becomes crucial; programs like Medicaid waivers under the HCBS often fill gaps, offering therapies without private insurance limits, especially for low-income households.
If your state falls short, start by contacting your insurer or the state insurance department to confirm coverage details–prior authorization may be required, and results may vary. We recommend consulting a healthcare professional for personalized guidance, as information here is not a substitute for professional medical advice. Exploring Does Insurance Cover ABA Therapy can clarify options further. At Heart Core ABA, our team handles insurance verification across Missouri and Illinois, coordinating with Medicaid and private plans to ease the process and focus on real progress through hands-on support.
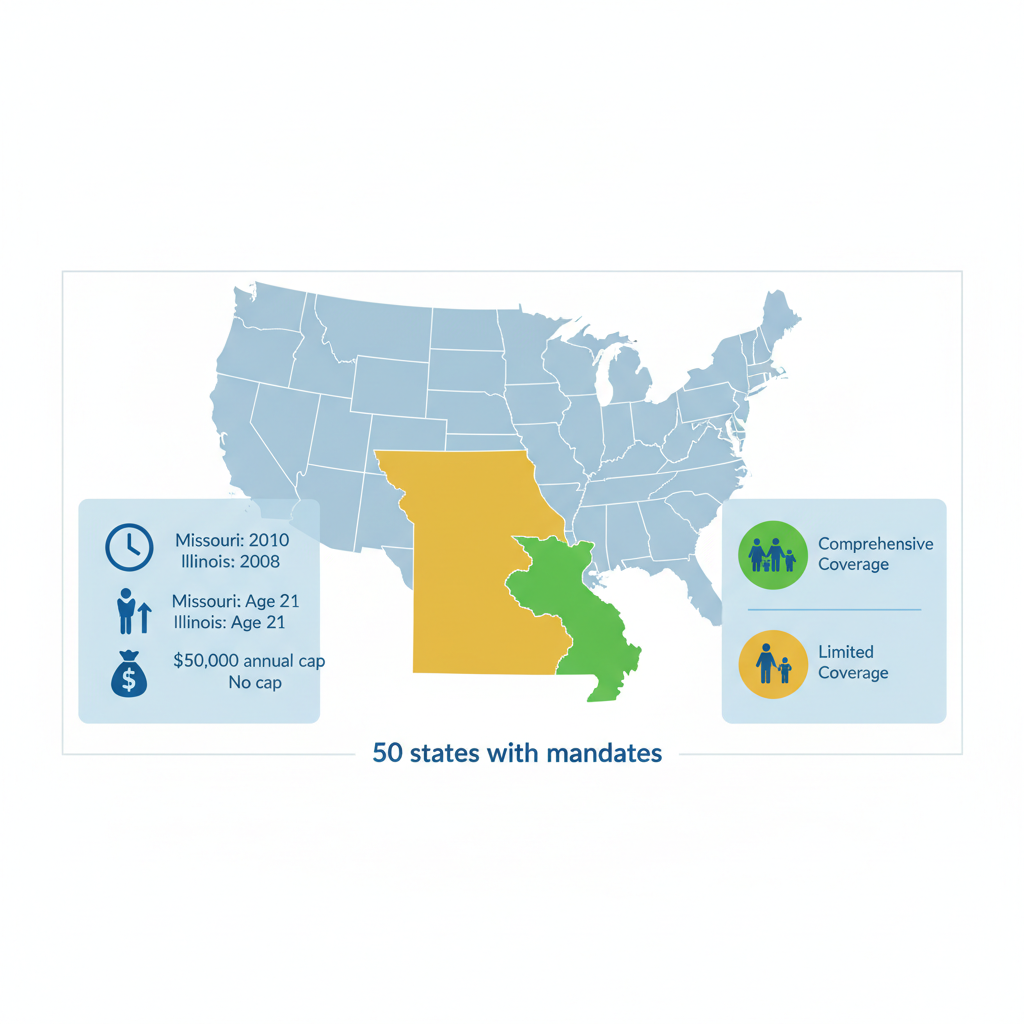
State variations in ABA insurance mandates across the US
This visual reinforces the geographic nuances, reminding us that while frustrations arise from inconsistencies, proactive steps like plan reviews lead to better connections with care that comes straight from the heart.
Navigating Insurance Verification for ABA Therapy
At Heart Core ABA, we understand how overwhelming it can feel to navigate insurance for ABA therapy. Many families in Missouri and Illinois wonder about does insurance cover aba therapy. We’re here to guide you through the verification process, helping you access the hands-on ABA therapy your child needs. This section breaks down the steps, documentation, and common hurdles to make benefit verification for behavioral therapy smoother. Remember, coverage may vary, so always verify your specific plan details.
Steps to Verify Your ABA Therapy Benefits
Verifying if aba therapy covered by insurance is essential for families seeking services in Missouri and Illinois. We guide families through these steps at Heart Core ABA, starting with understanding your policy basics. Begin by gathering your insurance card and any policy documents from your provider.
- Contact Your Insurer’s Member Services: Call the number on your insurance card to request a benefits summary. Ask about coverage for autism services, including ABA therapy. For private plans common in our region, this initial call often takes 1-2 days and provides an overview of in-network providers like us.
- Review Plan Details: Once you receive the summary, check for aba therapy insurance by state specifics, as Missouri and Illinois mandates differ slightly. Look for terms like authorization for autism services and any annual limits or copays.
- Speak with a Specialist: If needed, request to connect with a behavioral health coordinator. They can clarify eligibility for early intervention or school-based options we offer.
- Document Everything: Note dates, names, and reference numbers from your call. This helps if issues arise later.
According to Autism Speaks resources, starting verification early ensures timely access to care. For Medicaid plans, expect a longer initial outreach to state agencies, which can take 5-10 days. We at Heart Core ABA often assist with this first step to save you time.
The following table compares the verification process for private insurance versus Medicaid, highlighting key differences in timelines and requirements:
| Feature | Full Coverage States (e.g., IL) | Limited Coverage States |
|---|---|---|
| Hours per Week | Up to 40 | 10-20 |
| Age Eligibility | Birth to 21 | 3-18 |
This overview shows private plans often move faster, while Medicaid involves more structured screenings under EPSDT guidelines, which mandate coverage for necessary services as per Medicaid.gov. To save time, prepare documents in advance and consider our insurance verification assistance–many families report quicker resolutions when we handle the coordination. Overall, proactive steps like these reduce delays in starting personalized therapy plans.
Required Documentation and Prior Authorizations
Gathering the right paperwork is crucial for authorization for autism services through insurance. At Heart Core ABA, we help families compile these essentials to support claims for our in-home and center-based programs.
Key documents include a formal diagnosis of Autism Spectrum Disorder (ASD) from a qualified physician or psychologist, typically using DSM-5 criteria. You’ll also need a comprehensive functional behavioral assessment, outlining your child’s specific needs and how ABA therapy addresses them. For parent coaching or social skills groups, include any existing Individualized Education Program (IEP) details to show alignment with school goals.
Prior authorizations are standard for ABA claims. Submit these to your insurer within 30 days of diagnosis, as recommended by Autism Speaks checklists. Timelines vary: private insurers may approve in 2-4 weeks, while Medicaid processes under EPSDT can extend to 30-90 days, ensuring all medically necessary services are covered.
For aba therapy medicaid coverage in Missouri and Illinois, include an EPSDT screening form verifying developmental needs. We coordinate this with our BCBAs, who prepare detailed treatment plans emphasizing real progress through play-based methods. If out-of-pocket options arise, discuss private-pay rates with us–results may vary, and prior authorization may be required. Always consult your healthcare professional for personalized advice. Our team handles billing for major private plans and Medicaid, streamlining real connection with care that comes straight from the heart.
Appeals for denials require resubmitting with additional evidence, like updated assessments. We guide you here too, ensuring weekly parent updates keep you informed.
Common Challenges and How to Overcome Them
Families often face hurdles in verifying aba therapy medicaid coverage or private benefits. One common issue is vague policy language, leading to confusion about covered hours or provider networks. To overcome this, request a written explanation of benefits (EOB) and cross-reference with state guidelines–Missouri and Illinois resources clarify mandates.
Delays in prior authorizations frustrate many, especially with Medicaid’s longer EPSDT reviews. We mitigate this by submitting complete packets upfront and following up promptly. Another challenge is denials due to missing documentation; always double-check ASD diagnosis validity and include recent evaluations.
Out-of-pocket surprises occur if coverage falls short. Explore sliding-scale options or our family training sessions as bridges. Empathetically, we know these obstacles add stress–our insurance navigation support eases the load, fostering real progress. Verify coverage specifics, as plans differ, and reach out for help starting your journey.
Medicaid Coverage for ABA Therapy
At Heart Core ABA, we understand how crucial access to effective treatments like ABA therapy can be for children with autism. Medicaid plays a vital role in making aba therapy covered by medicaid more attainable for low-income families. Under federal law, Medicaid’s Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit requires coverage for all medically necessary services for children under 21, including ABA therapy as an evidence-based intervention for autism spectrum disorder (ASD). As outlined on Medicaid.gov, this mandate ensures states provide behavioral services without arbitrary limits, supporting developmental progress in social, communication, and daily living skills. According to the 2022 IACC Report to Congress, about 80% of states deliver these public autism therapy benefits through waiver programs, addressing the needs of the 1 in 44 children diagnosed with ASD.
Applying for aba therapy medicaid coverage involves verifying eligibility through your state’s Medicaid agency. In Missouri and Illinois, families can start by contacting the Department of Social Services or the Department of Healthcare and Family Services, respectively. We assist with Medicaid navigation by handling insurance verification and prior authorizations, which may be required to confirm benefits. For instance, low-income families qualify via income thresholds or Supplemental Security Income (SSI), and once approved, providers like us coordinate billing to streamline access. State waiver programs, such as Missouri’s Missouri MO HealthNet for Children or Illinois’ Medicaid Community-Based Services, expand options for in-home or center-based ABA, aligning with Individualized Education Programs (IEPs). This process typically takes 30-60 days, but our team guides families every step, ensuring personalized therapy plans fit within approved guidelines. Remember, while EPSDT covers essential services, copays may apply based on income, and results may vary–always consult your healthcare professional.
Coverage limits for ABA therapy vary by state, influencing aba therapy insurance by state. Typically, approved hours range from 20 to 40 per week, depending on the child’s needs and assessment. Age eligibility often spans from diagnosis to 21, though some states cap at 18. These variations highlight the importance of checking your state’s specifics to avoid gaps in care.
Drawing from Medicaid.gov and National Conference of State Legislatures (NCSL) data, full coverage states like Illinois offer more robust support through comprehensive waivers, while limited ones may restrict hours or age groups, potentially requiring supplemental private options. We recommend families contact their state agency or use tools like InsureKidsNow.gov to verify current benefits in your state. At Heart Core ABA, our insurance verification and Medicaid assistance help bridge these differences, delivering hands-on ABA therapy for children who learn differently with real progress and real connection. If prior authorization is needed, we’ll manage it to focus on care that comes straight from the heart.
Frequently Asked Questions on ABA Insurance
We often hear questions about aba therapy covered by insurance, especially for families in Missouri and nearby Illinois. Here are answers to some common concerns.
How can I check aba therapy insurance by state mandates?
Most states, including Missouri, require coverage for autism treatments like ABA under laws outlined by the National Conference of State Legislatures (NCSL). Check your state’s health department website or contact us at Heart Core ABA for guidance on autism therapy covered by insurance. We help verify benefits quickly.
Is ABA therapy free with Medicaid?
ABA therapy medicaid coverage varies, but under EPSDT standards from Medicaid.gov, eligible children get necessary services at little to no cost. It depends on your income and state plan–always verify eligibility first.
How do I apply for Medicaid ABA coverage?
Start by contacting your state Medicaid office for an application. Provide your child’s diagnosis and our BCBA assessment. We at Heart Core ABA assist with paperwork and prior authorizations to make it smoother.
What documentation is needed for insurance approval?
You’ll need a formal autism diagnosis, a treatment plan from a BCBA, and proof of medical necessity. Coverage queries for autism therapy often hinge on these–reach out to us for support.
Ready for next steps? Contact Heart Core ABA to explore your options today.
Accessing ABA Therapy Coverage
With ABA therapy covered by insurance now mandated in all 50 states, families gain vital access to essential support. We’ve explored how ABA therapy insurance by state shapes options, alongside ABA therapy Medicaid coverage for eligible households. Remember to verify your plan, gather documentation, and note state-specific tips for smooth approvals–prior authorization may be required.
We’re here to help at Heart Core ABA, offering hands-on guidance through insurance verification and personalized plans. Reach out today to explore your coverage and take the next step toward care that comes straight from the heart.
Your child’s real progress awaits. For more tools, visit Autism Speaks’ health insurance resources.















