ABA Therapy Covered By Medicaid
Table of Contents
Navigating Medicaid Coverage for ABA Therapy
Navigating insurance for your child’s care can feel overwhelming, especially when seeking early intervention for autism spectrum disorder. At Heart Core ABA, we understand how important it is to know that aba therapy covered by medicaid is an option in many cases, providing families with accessible support for skill development and behavioral progress. Our hands-on ABA therapy for children who learn differently focuses on real progress through personalized, play-based sessions delivered in-home, at school, or in our centers across Missouri and nearby Illinois communities. For details on how Medicaid supports ABA services, see ABA Therapy Medicaid.
Applied Behavior Analysis (ABA) therapy is an evidence-based approach that helps children with autism build essential skills like communication and social interaction. Under federal guidelines from the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) program referenced in Medicaid’s autism services resources, states like Missouri and Illinois implement coverage for these Medicaid-funded behavioral interventions. This means state-sponsored ABA programs can address developmental needs without financial strain for eligible families. Key factors for medicaid aba therapy eligibility often include a formal autism diagnosis and the child’s age, typically under 21. We at Heart Core ABA play a vital role by verifying benefits, handling prior authorizations, and coordinating care with our BCBA-led teams to ensure seamless access. Note that prior authorization may be required, and we recommend verifying your specific medicaid aba coverage by state with your provider.
To access these benefits, families must meet specific criteria–let’s explore those next, along with the steps for getting started and best practices for maximizing your coverage.
Key Eligibility Criteria for ABA Therapy Under Medicaid
Navigating eligibility for ABA therapy can feel overwhelming, but understanding the key criteria makes it more approachable. At Heart Core ABA, we specialize in guiding families through Does Medicaid Cover ABA Therapy to access essential services. Medicaid covers ABA therapy for qualifying children with autism spectrum disorder, often through the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit, which ensures comprehensive care. This federal mandate requires states like Missouri and Illinois to provide all medically necessary services. Let’s break down the main requirements to help you assess your family’s situation.
Diagnosis and Age Requirements
A primary step in medicaid aba therapy eligibility is a formal diagnosis of autism spectrum disorder (ASD) based on DSM-5 criteria, typically confirmed by a qualified physician or psychologist. This diagnosis establishes the medical necessity for ABA therapy covered by medicaid, focusing on behavioral interventions to address developmental delays, social skills deficits, and communication challenges. Age limits generally extend up to 21 years under EPSDT provisions, allowing coverage for adolescents transitioning to adulthood, though some states cap services earlier for non-early intervention cases.
In Missouri and Illinois, medicaid aba coverage by state aligns with these federal standards, with Missouri’s MO HealthNet emphasizing early diagnosis for toddlers and Illinois extending benefits through school age via waivers. For example, children diagnosed before age three in our service areas often qualify for qualifying for state-funded ABA without strict upper limits until 21.
We help families secure these evaluations by connecting them with trusted diagnosticians and starting with our early intervention programs, which use play-based activities to build foundational skills right away. Our BCBAs review diagnoses to ensure seamless integration into personalized therapy plans.
Income and Residency Qualifications
Medicaid eligibility hinges on family income thresholds, typically at or below 138% of the federal poverty level for children, with asset limits excluding primary homes and vehicles. This income-based qualification ensures access for low-to-moderate income households, while Medicaid behavioral therapy criteria also consider household size and additional factors like disabilities. Residency is straightforward: families must live in the state where applying, with no out-of-state coverage for routine services.
For our Missouri and Illinois communities, eligibility in Missouri requires enrollment in MO HealthNet, often through automatic qualification for Supplemental Security Income recipients, while coverage in Illinois falls under the state’s All Kids program with similar income caps around $3,000 monthly for a family of four. These regional notes reflect how medicaid aba coverage by state varies slightly but maintains core protections.
We assist by verifying income details during consultations and explaining residency proofs like utility bills. Our insurance navigation team handles applications to reduce barriers, focusing on real progress through accessible care that comes straight from the heart.
Documentation and Assessment Needs
Required documentation includes the ASD diagnosis report, proof of Medicaid enrollment, and functional behavior assessments (FBAs) conducted by Board Certified Behavior Analysts (BCBAs) to outline therapy goals. Prior authorization from Medicaid is common, involving medical necessity justification. For school-aged children, coordination with Individualized Education Programs (IEPs) strengthens cases, addressing developmental delays through targeted interventions.
In Missouri and Illinois, assessments follow EPSDT guidelines, with Illinois requiring comprehensive developmental screenings and Missouri mandating BCBA-led evaluations for waiver approvals. Common documents include physician referrals and income verification forms, submitted via state portals.
We streamline this by providing BCBA assessments at no initial cost and guiding families through a simple process:
- Gather diagnosis and Medicaid ID.
- Schedule our FBA to detail needs.
- Submit for prior authorization with our support.
Our IEP coordination ensures school-based ABA fits seamlessly, emphasizing personalized therapy plans. Remember, prior authorization may be required, and results may vary–always verify coverage with your provider.
Once eligible, families can access significant advantages–let’s explore those next.
Benefits of Medicaid Coverage for ABA Therapy
At Heart Core ABA, we understand how vital access to quality care can be for families navigating autism support. Aba therapy covered by medicaid opens doors to essential services without the heavy financial burden, especially in Missouri and Illinois. This coverage ensures children receive evidence-based interventions like Applied Behavior Analysis (ABA) therapy, promoting skill development and family well-being. We’re here to make this seamless, guiding you through verification and coordination.
Financial Relief and Accessibility
Medicaid brings significant financial relief by minimizing out-of-pocket costs for ABA therapy. Families often face low or no copays, making intensive 1:1 sessions affordable even in underserved areas. In Missouri and Illinois, this means broader access to services where providers might otherwise be scarce, allowing consistent therapy without travel hardships.
Aba therapy covered by medicaid extends to comprehensive plans under the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit, mandating coverage for medically necessary behavioral therapies for children under 21. This reduces barriers, enabling more families to prioritize treatment over budgeting concerns. Our team handles insurance verification, ensuring you maximize these benefits with personalized plans that fit your needs.
We focus on accessibility by offering in-home and community-based options, bringing hands-on ABA therapy right where it’s needed most. This approach not only cuts costs but also enhances participation, leading to real progress in daily skills.
Enhanced Family Support and Outcomes
Medicaid coverage shines in supporting families through integrated services like parent coaching and social skills groups. These elements foster stronger home environments, where caregivers learn techniques to reinforce therapy gains. For children, this translates to improved communication and independence, building on medicaid aba therapy eligibility criteria that prioritize early intervention.
Under EPSDT guidelines, states must provide all necessary treatments, including family training to address developmental needs holistically. Our BCBA-led teams deliver weekly updates and consistent RBT matches, ensuring therapy aligns with your child’s unique goals. Social skills groups covered by Medicaid help kids practice interactions in safe settings, boosting confidence and peer connections.
While results may vary, evidence-based ABA promotes measurable outcomes without promises of cures. We’re committed to real connection through caregiver coaching, helping families feel empowered. This comprehensive support enhances overall family dynamics, making therapy a collaborative journey toward better skill development.
State-Specific Advantages in MO and IL
Missouri and Illinois offer tailored Medicaid advantages for ABA therapy, integrating with Individualized Education Programs (IEPs) for seamless school support. In Missouri, coverage emphasizes flexible hours tied to assessments, while Illinois highlights early intervention perks. Both states align with EPSDT to cover birth to age 21, but nuances in service delivery affect planning.
Understanding medicaid aba coverage by state helps families navigate regional therapy funding perks. Missouri prioritizes in-home and school-based options, often linking directly to IEPs for educational continuity. Illinois extends similar benefits with added focus on group therapies, ensuring comprehensive access across settings.
Our role involves coordinating prior authorizations and matching services to state guidelines, maximizing benefits of Medicaid ABA support. We provide BCBA supervision to meet hour limits without gaps, supporting IEP integrations for holistic care.
The following table outlines key differences to clarify these variations:
| Aspect | Missouri | Illinois |
|---|---|---|
| Hourly Limits | Up to 40 hours/week based on assessment | Similar, with emphasis on early intervention |
| Age Coverage | Birth to 21 via EPSDT | Birth to 21 via EPSDT |
| Service Types | In-home, school, center-based | Includes social skills groups |
| Prior Auth Requirements | Annual renewals | Annual renewals |
These state variations reflect flexible implementations of federal EPSDT mandates, ensuring behavioral therapies like ABA are accessible yet adapted to local needs. Sourced from state Medicaid guidelines, the table highlights how Missouri and Illinois balance coverage scopes for optimal family support.
At Heart Core ABA, we navigate these differences by verifying eligibility and securing approvals upfront. Our insurance assistance streamlines access, whether in Missouri or Illinois, so you can focus on your child’s progress. With personalized therapy plans and family training, we turn these advantages into actionable care–verify your coverage today, as prior authorization may be required.
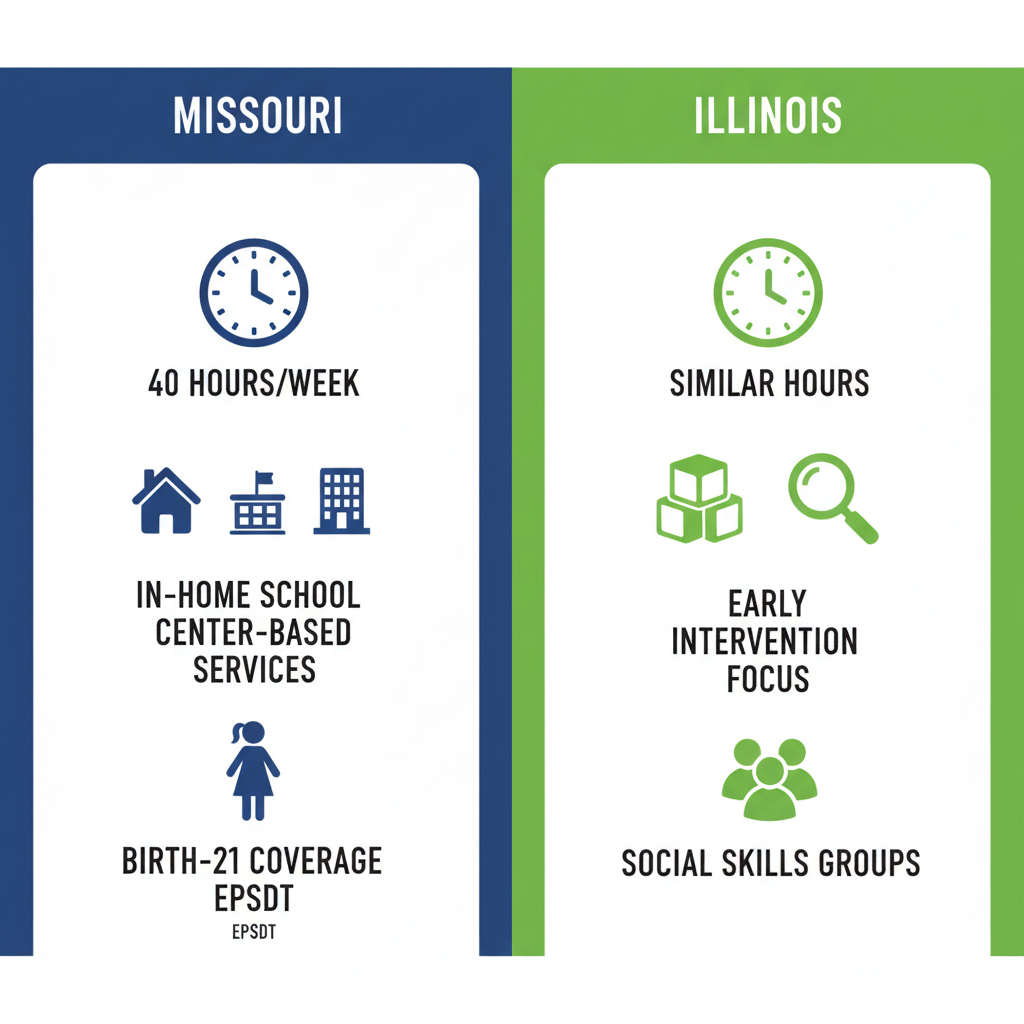
Medicaid ABA therapy coverage comparison: Missouri vs. Illinois
This visual underscores the shared commitment to early intervention, helping families in our communities make informed choices. Understanding these benefits leads to knowing how coverage works in practice–next up.
How Medicaid ABA Therapy Coverage Works
Navigating Medicaid coverage for ABA therapy can feel overwhelming, but we’re here at Heart Core ABA to guide you every step of the way. Our team specializes in hands-on ABA therapy for children who learn differently, ensuring real progress through personalized plans. With a focus on Missouri and Illinois, we help families understand the process, from initial applications to ongoing support, so your child receives the care that comes straight from the heart. Remember, while we assist with verification, always verify insurance coverage and that prior authorization may be required.
Application and Prior Authorization Process
Applying for Medicaid ABA therapy starts with ensuring your child meets the basics for eligibility, often tied to a diagnosis like autism spectrum disorder. Under the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit, Medicaid in Missouri and Illinois covers comprehensive services for kids under 21, including aba therapy covered by medicaid when medically necessary. Here’s a step-by-step guide:
- Enroll in Medicaid through state portals like mydss.mo.gov for Missouri or abe.illinois.gov for Illinois. Gather documents such as income proof, birth certificates, and medical records showing your child’s needs.
- Once enrolled, request a screening via EPSDT, which includes developmental assessments to identify behavioral therapy requirements.
- Submit prior authorization for ABA services, including a BCBA assessment report outlining treatment goals. This goes to the state Medicaid agency, typically within 30 days federally mandated timelines.
In Missouri, use the MO HealthNet system for faster processing, while Illinois requires forms through the Department of Healthcare and Family Services. Why it matters: These steps unlock essential early intervention, aligning with IEPs for school-aged kids. Pro tip: We handle insurance verification upfront, saving you time and reducing stress–contact us to start.
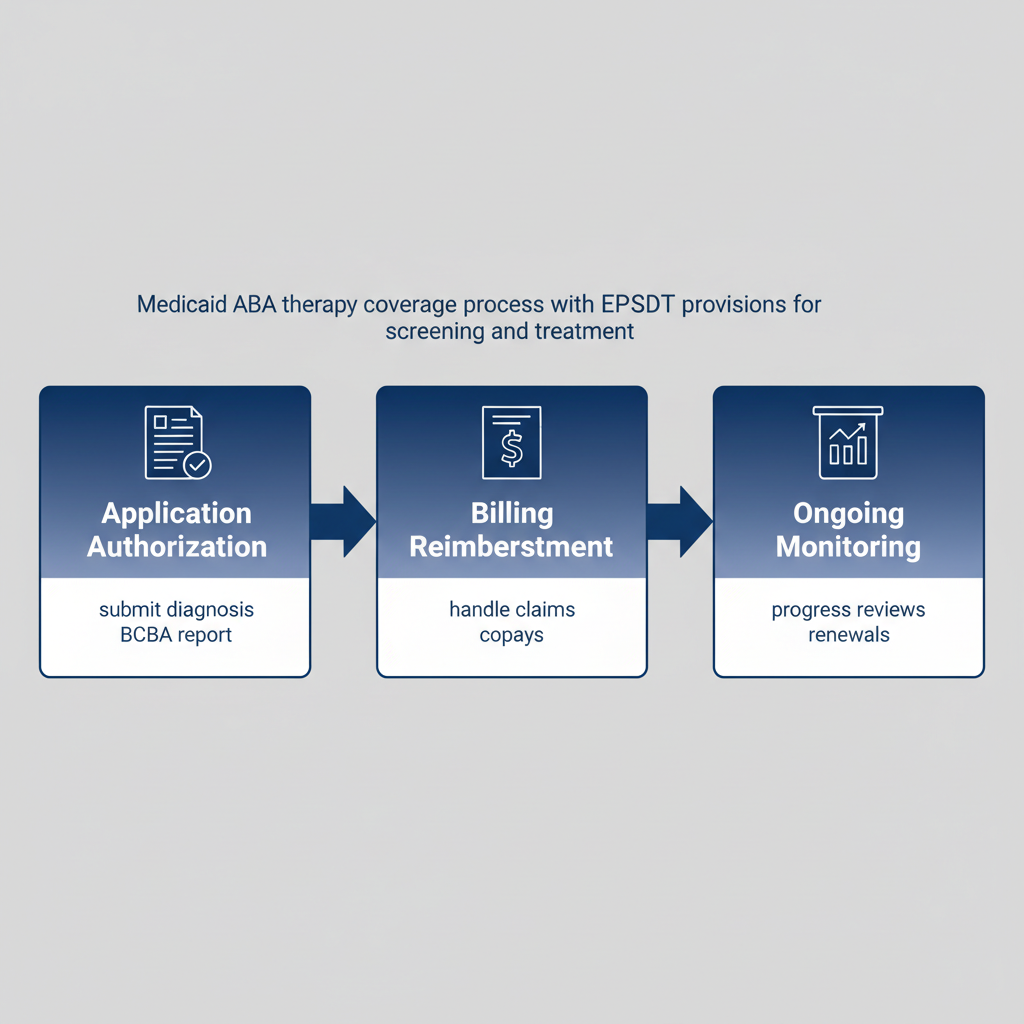
Process flow for Medicaid ABA therapy coverage steps
This visual outlines the journey, helping families visualize each phase. Building on a smooth application, the next areas focus on sustaining coverage through billing and adjustments.
Billing and Reimbursement Details
Once approved, billing for ABA therapy follows structured medicaid aba coverage by state guidelines, with providers like us managing claims to minimize family out-of-pocket costs. We coordinate with Medicaid in Missouri and Illinois, processing reimbursements for services such as in-home 1:1 RBT-delivered therapy and BCBA supervision.
Claims are submitted electronically via state portals, with typical processing in 45-60 days per federal EPSDT rules. Copays, if any, are capped low–often $0 to $4 per visit–and waived for many low-income families. For dual coverage, we handle coordination with private insurance first, then Medicaid as secondary payer, ensuring no double billing.
Medicaid claim procedures for ABA involve detailed coding for sessions, like parent coaching or social skills groups. In Illinois, use the IMPACT system for tracking, while Missouri’s emphasizes timely state reimbursement for behavioral therapy. This keeps therapy affordable and focused on progress.
Our role: We verify benefits, bill accurately, and provide transparent updates weekly. Tip: Keep records of sessions to support claims, and reach out if delays occur–we advocate for you.
Ongoing Monitoring and Adjustments
Medicaid aba therapy eligibility requires regular check-ins to maintain coverage, emphasizing progress reports and renewals under EPSDT’s periodic screening mandates. We support this by aligning therapy with IEPs, adjusting goals based on your child’s advancements in skills like communication or daily routines.
Annual reviews involve BCBA-led assessments submitted for reauthorization, typically every 6-12 months depending on state rules. In Missouri and Illinois processes, these include data from sessions showing measurable outcomes, ensuring continued medical necessity.
If needs change, we update plans promptly–perhaps adding early intervention for toddlers or school-based services. Why it matters: Ongoing monitoring prevents coverage gaps, fostering real connection and sustained growth.
We guide families through renewals, offering family training to track home progress. Pro tip: Document milestones to strengthen reports; our team coordinates with schools for seamless IEP ties. For more on does medicaid cover aba therapy, explore our resources. With these mechanics in place, families can optimize their experience by staying proactive and partnered with us.
Best Practices for Securing Medicaid ABA Coverage
Navigating Medicaid for ABA therapy can feel overwhelming, but with the right steps, families in Missouri and Illinois can optimize their access to essential support. At Heart Core ABA, we prioritize family collaboration and insurance assistance to make this process smoother. These best practices draw from federal guidelines on autism services, helping you prepare effectively and build strong partnerships.
Preparing Documentation and Applications
We recommend starting with a comprehensive gathering of medical records to ensure your application for aba therapy covered by medicaid stands strong. Timely diagnosis documentation is key; secure a formal autism spectrum disorder evaluation from a qualified professional early on. This sets the foundation for proving medical necessity. For additional guidance on what Medicaid covers and next steps, visit aba therapy medicaid.
Here are actionable steps to streamline your submission:
- Collect all relevant records: Include doctor’s notes, developmental assessments, and any prior therapies to demonstrate eligibility.
- Complete forms accurately: Double-check for Missouri or Illinois-specific requirements, like prior authorization details, to avoid delays.
- Consult a BCBA early: Their input can strengthen your case by outlining a personalized therapy plan.
These practices work because they align with federal appeals guidelines, reducing rejection risks through thorough evidence. For instance, families who’ve submitted complete packets in our regions often see approvals within weeks. We assist by verifying benefits at no initial cost, guiding you through paperwork so you focus on your child’s progress. This approach not only speeds up access but also integrates our play-based methods from the start.
Working with Providers Like Heart Core ABA
Partnering with credentialed providers transforms the Medicaid process into a collaborative journey. In Missouri and Illinois, understanding medicaid aba coverage by state variations is crucial, as each has unique verification timelines and documentation needs. We at Heart Core ABA specialize in these nuances, offering hands-on support for smooth implementations.
Key strategies for effective collaboration include:
- Choose BCBA-led teams: Look for providers with experienced analysts who handle authorizations and tailor plans to IEPs.
- Request consistent RBT assignments: This ensures familiarity and real progress through steady 1:1 sessions.
- Leverage parent coaching: Regular updates help track therapy hours and adjust as needed.
Working this way builds trust and efficiency; for example, our weekly family trainings have helped Missouri families coordinate school-based services seamlessly. Our unique selling point is BCBA supervision paired with consistent RBT matches, plus insurance navigation that covers prior authorizations. Remember, while we assist extensively, always verify coverage details directly, as requirements can vary.
Addressing Common Challenges and Misconceptions
Challenges like denials or partial coverage arise, but proactive strategies can resolve them. Many wonder about medicaid aba therapy eligibility beyond Missouri and Illinois–note that while Texas has its own rules, focusing on state-funded therapy here means checking local caps on hours. Misconceptions, such as assuming universal full coverage, often lead to frustration; in reality, results may vary based on individual plans.
Effective tactics to overcome hurdles:
- File appeals promptly: Use federal guidelines to document medical necessity, citing successful state examples for stronger cases.
- Coordinate with schools: Align IEPs to support therapy extensions and clarify partial costs, like copays for extras.
- Track hours with tools: Apps or logs help monitor usage and prepare for renewals.
These steps empower you by addressing root issues head-on; one Illinois family overturned a denial through our guidance on appeals, gaining full-session access. We provide empathetic support, debunking myths while emphasizing no guarantees–consult professionals for specifics. By tackling these, you’re better equipped for ongoing success.
By following these practices, you’re set for success–let’s summarize key takeaways in our next section.
Taking the Next Step in ABA Therapy Access
Navigating aba therapy covered by medicaid can open doors to essential support for children with autism in Missouri and Illinois. We’ve covered the basics of medicaid aba therapy eligibility, which generally requires a diagnosis of autism spectrum disorder and enrollment in state Medicaid programs. In Missouri, families benefit from comprehensive coverage including assessments and ongoing sessions, while Illinois emphasizes early intervention through its programs. Understanding medicaid aba coverage by state helps secure these vital resources, though partial coverage may mean out-of-pocket costs for some services.
At Heart Core ABA, we’re dedicated to easing these barriers with our hands-on ABA therapy for children who learn differently. Our team handles insurance verification and coordinates prior authorizations, including guiding families through options for aba therapy covered by insurance, ensuring you focus on your child’s real progress and real connection. We offer personalized therapy plans, whether in-home, school-based, or center-based, delivered by our BCBA-led teams with consistent RBT support. Remember, results may vary, and prior authorization may be required–always verify your coverage.
Ready to start? Contact us today–we’re ready to help with a free consultation to explore securing Medicaid for behavioral therapy and your regional ABA funding summary. The Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit under Medicaid provides a strong foundation for these services. Together, we can support your child’s growth through care that comes straight from the heart.















