Autism Therapy Covered By Insurance
Table of Contents
Navigating Autism Therapy Insurance Coverage
We know how overwhelming it can feel to seek autism therapy covered by insurance in Missouri or nearby Illinois communities, especially when your child needs early intervention. At Heart Core ABA, we’ve helped countless families navigate this process, verifying benefits to make hands-on ABA therapy for children who learn differently more accessible and affordable.
Applied Behavior Analysis (ABA) therapy is a evidence-based treatment that breaks down skills into manageable steps, using positive reinforcement to support children with autism spectrum disorder in developing communication, social, and daily living abilities. For guidance on insurance specifics and coverage options, see ABA Therapy Covered By Insurance. Under the Affordable Care Act, many health plans must cover autism treatments like ABA, though specifics vary by state. For instance, autism insurance coverage by state often includes mandates for aba therapy insurance coverage, with benefit caps and prior authorizations as common requirements. Medicaid plays a key role too, offering support for eligible families. Our team at Heart Core ABA handles benefit verifications and coordinates with insurers, ensuring personalized therapy plans delivered by credentialed BCBAs and RBTs.
In the sections ahead, we’ll dive deeper into understanding your coverage, exploring benefits, guiding you through the claims process, and sharing best practices for success. Remember, prior authorization may be required, and we recommend verifying your plan details with your provider to ensure the best fit for your family’s needs.
Understanding ABA Therapy and Insurance Basics
What ABA Therapy Entails and Why Insurance Matters
We often see families wondering about the path forward when a child receives an autism diagnosis, and that’s where ABA therapy comes in. Applied Behavior Analysis, or ABA, is an evidence-based intervention that focuses on building essential skills through positive reinforcement and hands-on techniques tailored to each child’s needs. It targets areas like communication, social interactions, and daily routines, helping kids who learn differently make real progress in their own way. At Heart Core ABA, our hands-on ABA therapy for children who learn differently emphasizes play-based learning to foster real connection and care that comes straight from the heart.
Insurance plays a pivotal role in making this accessible, especially since ABA can involve ongoing sessions that add up financially. Under the Affordable Care Act’s Section 5113, many plans must cover autism therapy covered by insurance, but state laws fill in the gaps to ensure families aren’t left navigating costs alone. For us in Missouri and nearby Illinois communities, understanding coverage for behavioral interventions means more families can access in-home or school-based services without undue burden. We handle insurance verification to simplify this, but remember, results may vary, and verifying insurance coverage is key–prior authorization may be required. This foundational support not only eases financial stress but also allows focus on what matters: your child’s personalized therapy plan.
State Variations in Autism Insurance Mandates
Navigating autism insurance coverage by state can feel like comparing regional traffic laws–rules differ, but knowing them helps everyone get where they need to go safely. Across the US, mandates stem from state laws building on federal guidelines, with some states requiring full coverage for ABA while others offer partial protections. In Missouri, for instance, HB 1734 established a partial mandate via state law, meaning certain plans cover ABA therapy in Missouri communities up to specific limits. Illinois, on the other hand, enforces a full mandate with comprehensive coverage, ensuring broader access for families there.
These differences highlight why state autism benefits policies vary so much–what’s standard in one place might require extra steps in another. To illustrate, here’s an overview of key variations in select states, drawing from established guides like the State-by-State Guide to Autism Insurance Laws:
| State | Mandate Status | Age Limit | Annual Cap Example |
|---|---|---|---|
| Missouri | Partial mandate via state law | Up to age 19 | Varies by plan |
| Illinois | Full mandate | Up to age 21 | Medically necessary |
This table underscores how mandates shape access, with Illinois offering more expansive protections compared to Missouri’s targeted approach. Families should always check their specific plan details, as expansions in Medicaid can further influence availability. We recommend consulting your provider or a specialist to confirm what’s covered under your policy.
Building on these state differences, visual aids can clarify the landscape even more, showing how age limits and caps impact planning for long-term care.
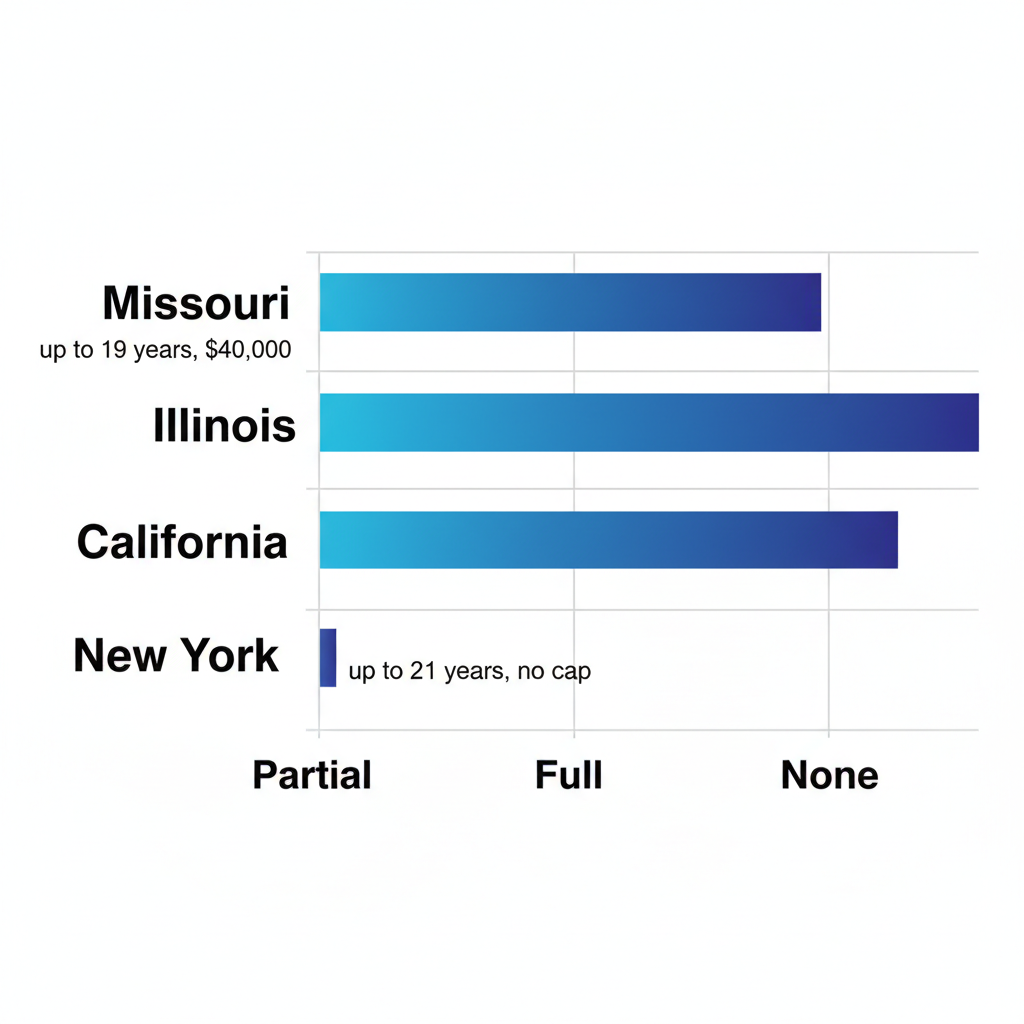
State-by-state overview of autism insurance mandates for ABA therapy
Such illustrations remind us that while policies evolve, proactive steps like reviewing annual reports from autism advocacy groups keep families informed and empowered.
Eligibility Criteria for Coverage
When it comes to aba therapy insurance coverage, eligibility starts with a clear diagnosis and meeting plan-specific rules–we’re here to guide families through this every step. First, a qualified professional must diagnose autism spectrum disorder using DSM-5 criteria, often involving assessments from a developmental pediatrician or psychologist. This formal diagnosis serves as the foundation, proving medical necessity for ABA as a behavioral intervention.
Next, age plays a role; many states cap coverage up to 21, though some like Illinois extend further, aligning with ongoing needs during school years. Plans may require additional documentation, such as a letter of medical necessity from the prescribing doctor outlining how ABA fits the child’s IEP or daily challenges. Employer-sponsored or commercial plans often follow these steps, while Medicaid expansions in Missouri provide another avenue for qualifying families.
Here’s a quick breakdown of common prerequisites:
- Obtain a DSM-5 autism diagnosis from a licensed clinician.
- Secure a prescription or recommendation for ABA therapy.
- Submit prior authorization requests with supporting assessments.
- Verify plan type–commercial, Medicaid, or employer–for state-specific mandates.
For more on this, explore Does Insurance Cover ABA Therapy. Keep in mind, information here isn’t a substitute for professional medical advice; always consult your healthcare team to tailor to your situation.
Key Benefits of Insurance-Covered Autism Therapy
At Heart Core ABA, we see firsthand how autism therapy covered by insurance opens doors for families seeking support for their children. This coverage not only eases financial pressures but also ensures consistent, hands-on ABA therapy for children who learn differently. By aligning with state mandates, it promotes real progress through personalized plans that foster real connections and care straight from the heart.
Financial Relief and Accessibility
Insurance coverage transforms the landscape of ABA services by significantly reducing out-of-pocket expenses for families across the US. Typically, plans cover up to 80% of therapy costs, meaning a session that might run $100-$200 privately could drop to just a $20 copay with benefits in place. This financial relief makes autism therapy covered by insurance a game-changer, enabling broader access to essential interventions without the burden of full private pay.
We believe this support extends nationwide, though generosity varies by location. For instance, in states like Missouri, partial requirements still offer substantial aid, while Illinois mandates no annual caps on benefits. According to state-by-state guides, such policies ensure low-income families can tap into Medicaid for aba therapy insurance coverage, covering early intervention for toddlers and ongoing sessions. This often leads to 20-40 hours of weekly therapy, far more than self-funded options allow. Ultimately, it democratizes access, helping more children receive the school-based or in-home ABA therapy they need to thrive.
Improved Outcomes Through Consistent Therapy
Sustained ABA intervention, backed by insurance, drives meaningful skill development in communication, socialization, and daily living for children on the autism spectrum. Evidence shows that consistent sessions–often 15-20 hours per week enabled by coverage–yield better results than sporadic therapy. At our centers, we witness how this continuity in aba therapy insurance coverage supports steady progress, from mastering social skills groups to enhancing IEP coordination.
Benefits of insured behavioral therapy include measurable gains, with studies indicating up to 47% improvement in adaptive behaviors when therapy is uninterrupted. Without financial barriers, families in US regions can commit to long-term plans supervised by our BCBAs, ensuring RBT-delivered 1:1 instruction aligns with each child’s needs. State-funded autism support plays a key role here; for example, robust coverage in progressive states allows for extended durations, often beyond the 2-3 years typical without insurance. We emphasize that while results may vary, this structure fosters real connection and personalized growth, verifying coverage to maximize every opportunity.
Family Support and Reduced Stress
Autism insurance coverage by state not only funds therapy but also bolsters family dynamics through inclusive services like parent coaching and caregiver training. In Missouri and nearby Illinois communities, these benefits reduce stress by integrating family involvement into treatment plans, helping parents build skills alongside their child. This collaborative approach at Heart Core ABA eases the emotional load, as covered sessions allow for weekly updates and hands-on guidance without added costs.
Key advantages include lower burnout rates for caregivers, with insurance enabling access to social skills groups and center-based programs that strengthen home environments. For low-income households, Medicaid assistance covers prior authorizations, ensuring no gaps in support–though annual maximums may apply in some areas, like Missouri’s limits versus Illinois’ open policies. We often hear from families how this state-funded autism support transforms daily life, promoting well-being and reducing isolation. Remember, verify your insurance coverage, as prior authorization may be required. With these benefits in mind, let’s see how coverage actually works.
How Insurance Coverage for ABA Therapy Works
Knowing the advantages of ABA therapy is great–now let’s walk through the how. At Heart Core ABA, we handle much of this for families, but understanding the process empowers you to navigate it confidently. This section breaks down verification, documentation, and coverage variations, focusing on procedures for therapy funding in Missouri and nearby areas.
The Verification and Authorization Process
Start by checking if aba therapy covered by insurance applies to your plan–it’s a key first step for autism therapy covered by insurance. We recommend calling your insurer or logging into their online portal to verify benefits. Ask about coverage for ABA services, including session limits, deductibles, and copays. For example, a sample script could be: “Does my plan cover Applied Behavior Analysis for autism under the age of 21, and what are the prior authorization requirements?”
Next, obtain prior authorization. This typically involves our Board Certified Behavior Analyst (BCBA) conducting an initial assessment to demonstrate medical necessity. Submit the request through the insurer’s preferred method, which might take 1-4 weeks. In Missouri, employer-sponsored plans often follow state mandates similar to EPSDT guidelines, ensuring timely access. We coordinate this at Heart Core ABA, submitting functional behavior assessments and treatment recommendations to streamline approval. Common pitfalls include incomplete submissions, so double-check details. Once approved, therapy can begin, with ongoing reviews every six months to confirm progress.
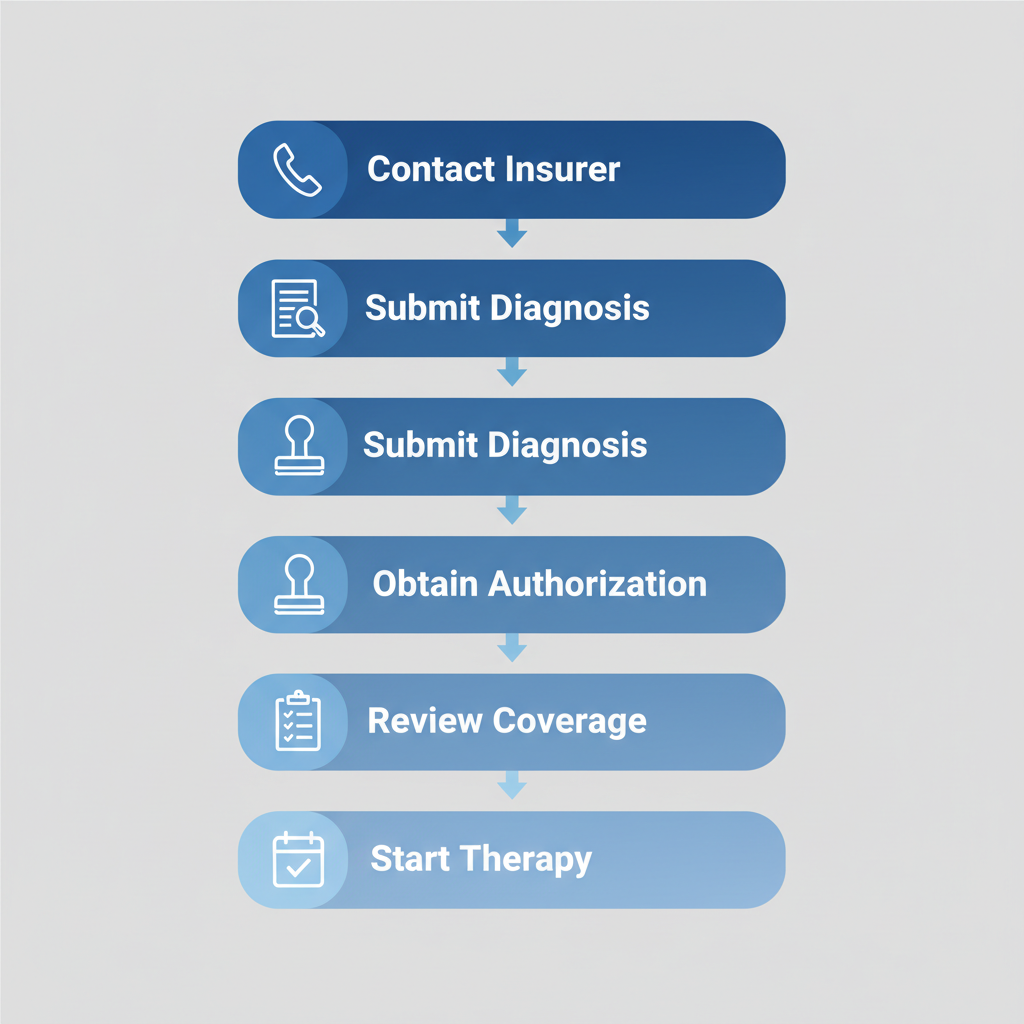
Steps for ABA therapy insurance verification and authorization process
This visual outlines the flow, helping families see how each step connects to real progress in personalized therapy plans.
Documentation and Medical Necessity Requirements
Gathering the right paperwork is crucial for ABA therapy insurance coverage approval. Begin with a formal autism diagnosis from a qualified physician, often including DSM-5 criteria and supporting reports. You’ll also need an Individualized Education Program (IEP) if your child is school-aged, highlighting how ABA aligns with educational goals.
Essential documents include a comprehensive functional assessment by a BCBA, detailing behaviors targeted for intervention, and a detailed treatment plan outlining goals, methods, and expected outcomes–like improving social skills through 1:1 RBT sessions. Medical necessity is proven by showing how ABA addresses core deficits in communication and daily living. In Missouri, insurers may require additional forms like prescription referrals. We assist families in compiling these, ensuring everything meets regional coverage protocols. Remember, results may vary, and consult a healthcare professional for personalized advice. This thorough preparation minimizes denials and gets therapy started sooner.
Coverage Under Different Plans and Medicaid
Coverage for ABA varies by plan type, with commercial and employer options often providing solid support under state laws. Private insurers typically cover up to 40 hours weekly for children under 21, subject to deductibles and copays. Employer plans might offer enhanced benefits through group policies, but always confirm aba therapy insurance coverage specifics.
Medicaid in Missouri expands access via EPSDT services, mandating coverage for necessary treatments without age caps in many cases. Eligibility involves income verification and state waivers, making it ideal for qualifying families. Autism insurance coverage by state differs–Missouri’s protocols emphasize early intervention, often with fewer barriers than commercial plans. For instance, Medicaid may waive copays based on income, funding in-home and school-based sessions. We verify Medicaid benefits and handle billing to simplify this. While private plans provide flexibility, public options ensure equity; choosing depends on your situation. Verify insurance coverage, as prior authorization may be required.
When selecting a plan, consider factors like session caps and provider networks–commercial insurance often has broader choices, while Medicaid prioritizes accessibility in underserved areas. The following table highlights key differences to aid your decision:
| Aspect | Commercial Insurance | Medicaid |
|---|---|---|
| Prior Auth Time | 1-4 weeks | 1-2 weeks in mandated states |
| Copay Typical | 20-50% | Low or none |
Commercial plans suit families with robust employer benefits, offering quicker specialist access, whereas Medicaid provides comprehensive support for lower-income households, aligning with Missouri’s commitment to early autism care. At Heart Core ABA, our team offers free insurance verification to match you with the best option, coordinating everything from assessments to ongoing billing. This guidance helps avoid surprises and focuses on real connection through care that comes straight from the heart.
Best Practices for Maximizing Autism Therapy Insurance Benefits
With the insurance process laid out, let’s dive into pro tips for success. At Heart Core ABA, we help families in Missouri and Illinois make the most of their coverage for personalized services like early intervention and social skills groups. These strategies can empower you to access the care your child needs without unnecessary roadblocks.
Preparing Documentation and Appeals
Start early by organizing key documents to support your claim for autism therapy covered by insurance. Gather updated Individualized Education Programs (IEPs), diagnostic reports from qualified professionals, and proof of medical necessity. We recommend creating a dedicated folder for all paperwork, including session notes and progress reports, to streamline submissions.
If a claim is denied, don’t hesitate to appeal. Begin with a clear letter outlining why the therapy is essential, referencing your policy’s terms. For example:
- State the denial and request a review.
- Attach supporting documents like doctor recommendations.
- Explain how ABA aligns with covered treatments.
Appeals succeed in many cases, especially with strong evidence. Remember, prior authorization may be required, so verify your benefits first. This preparation can help optimize therapy benefits and reduce out-of-pocket costs for aba therapy insurance coverage.
Navigating State-Specific Limits
Autism insurance coverage by state varies, so understanding local rules is key for state policy navigation tips. In Illinois, as a fully mandated state, coverage often includes no age cap for essential therapies, allowing continued support into adulthood. Missouri, with partial mandates, typically caps benefits at age 19 or around $40,000 annually, but extensions are possible through appeals.
To manage these limits:
- Track session hours against your cap using provider statements.
- Explore supplemental funding like Medicaid waivers for gaps.
- Plan transitions to adult services before age limits hit.
These steps address common questions like age limits for insurance coverage of autism therapy and finding state-specific benefits. By staying proactive, families can extend access to hands-on ABA therapy for children who learn differently.
The following table outlines common coverage limits and workarounds by state category, based on reliable state-by-state guides:
| State Type | Typical Limit | Best Practice |
|---|---|---|
| Mandated (e.g., IL) | No age cap | Leverage full benefits |
| Partial (e.g., MO) | Age 19 cap | Appeal for extensions |
This overview highlights how Illinois offers broader access compared to Missouri’s constraints. For instance, mandated states like Illinois ensure fuller coverage without strict annual dollars, while partial ones require creative advocacy. Always check your policy, as rules evolve–consult resources like state autism insurance laws for the latest.
Partnering with Providers for Support
Collaborating with experienced ABA providers like us at Heart Core ABA makes a big difference in verification and optimization. We handle insurance navigation, from initial benefit checks to billing Medicaid and major private plans, ensuring real progress through real connection.
Ask these questions when selecting a partner:
- How do you verify coverage and coordinate prior authorizations?
- Can you provide detailed session reports for appeals?
- What support do you offer for cap management or denials?
Our team, with BCBAs and RBTs, delivers consistent 1:1 therapy and IEP coordination. We support families through these steps every day, offering weekly updates and caregiver coaching to build care that comes straight from the heart. While results may vary, partnering this way often uncovers hidden benefits and smooths the path. Verify your insurance coverage with us today to see how we can tailor a personalized therapy plan.
For more on this, explore does insurance cover aba therapy. Information here is not a substitute for professional medical advice–consult your healthcare provider.
Securing Your Child’s Autism Therapy Path
As we’ve covered throughout this guide, navigating autism therapy covered by insurance can pave a clear path to insured autism support for your child’s development. From understanding mandates and documentation requirements to exploring benefits like aba therapy insurance coverage and autism insurance coverage by state, each family’s situation is unique–no two plans are identical. We’ve highlighted key practices, such as verifying eligibility for aba therapy covered by medicaid, gathering necessary medical records, and appealing denials when needed. These steps ensure access to vital ABA services in Missouri and Illinois, supporting skill-building and family well-being.
To take the final steps for coverage access, start by contacting your insurer for a personalized benefits review–remember, prior authorization may be required, and results may vary. At Heart Core ABA, we’re here to help you every step: we handle insurance verification, coordinate with Medicaid, and provide family training to maximize outcomes. Here’s how to move forward:
- Schedule a free consultation with our team to discuss your child’s needs.
- Reach out to resources like health insurance assistance organizations for advocacy support.
- Collaborate with your care team for integrated therapy plans.
With proactive effort and our collaborative care, you’ll empower your child toward real progress and brighter possibilities. Contact us today in Missouri or Illinois–we’re committed to care that comes straight from the heart.















